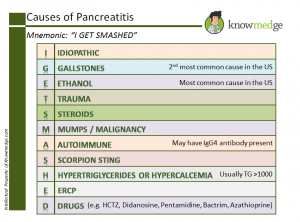
I Get Smashed Pancreatitis: Understanding And Managing This Serious Condition
Have you ever experienced severe abdominal pain that left you doubled over and wondering what could be wrong? If you've heard the term "i get smashed pancreatitis" and are curious about what it means, you're not alone. This alarming condition affects thousands of people each year and can be life-threatening if not properly managed.
Pancreatitis occurs when the pancreas becomes inflamed, causing severe pain and potentially serious complications. When we talk about "getting smashed" in relation to pancreatitis, we're typically referring to the intense, debilitating pain that patients describe as feeling like they've been physically hit or "smashed" in the abdomen. This pain is often accompanied by other distressing symptoms that can significantly impact quality of life.
What Exactly Is Pancreatitis?
Pancreatitis is an inflammatory condition of the pancreas, a vital organ located behind the stomach that produces digestive enzymes and hormones like insulin. When the pancreas becomes inflamed, these digestive enzymes can activate prematurely within the organ itself, essentially causing the pancreas to begin digesting its own tissue. This process leads to the characteristic severe pain and other symptoms that patients experience.
- Eva Violet Nude
- Exposed Janine Lindemulders Hidden Sex Tape Leak What They Dont Want You To See
- The Sexy Side Of Baccarat Leaked Methods To Win Big On Baccaratnet
The condition can manifest as either acute pancreatitis, which appears suddenly and typically resolves with treatment, or chronic pancreatitis, which develops gradually and causes persistent inflammation and damage over time. Both forms can be extremely painful and require medical attention, though acute pancreatitis often presents the most dramatic symptoms that patients describe as feeling "smashed."
Common Causes and Risk Factors
Understanding what triggers pancreatitis is crucial for prevention and management. The most common causes include:
Gallstones are the leading cause of acute pancreatitis, accounting for approximately 40-70% of cases. These small, hardened deposits can block the pancreatic duct, preventing digestive enzymes from reaching the small intestine and causing them to back up into the pancreas.
- Ross Dellenger
- Iowa High School Football Scores Leaked The Shocking Truth About Friday Nights Games
- Facebook Poking Exposed How It Leads To Nude Photos And Hidden Affairs
Alcohol consumption represents another major risk factor, particularly for chronic pancreatitis. Heavy alcohol use can cause the pancreas to produce toxic compounds that damage pancreatic tissue. Studies show that alcohol-related pancreatitis accounts for about 30% of acute cases and is the primary cause of chronic pancreatitis.
Other contributing factors include high triglyceride levels, certain medications, abdominal trauma, genetic predisposition, and autoimmune conditions. In some cases, the cause remains unknown, classified as idiopathic pancreatitis.
Recognizing the Symptoms: When You Feel "Smashed"
The hallmark symptom of pancreatitis is severe abdominal pain that patients often describe as feeling like they've been "smashed" or hit in the upper abdomen. This pain typically:
- Begins suddenly and intensifies over time
- Centers in the upper abdomen, often radiating to the back
- Worsens after eating, particularly fatty foods
- May be accompanied by nausea, vomiting, and fever
- Can cause the abdomen to become tender to touch
Additional symptoms may include rapid pulse, low blood pressure, and in severe cases, signs of shock. The pain can be so intense that patients find it difficult to find a comfortable position and may pace or writhe in discomfort.
Diagnosis and Medical Evaluation
When someone presents with symptoms suggesting pancreatitis, healthcare providers follow a systematic approach to diagnosis. This typically includes:
Blood tests to measure pancreatic enzyme levels, particularly amylase and lipase. Levels that are three times higher than normal strongly suggest acute pancreatitis. Other blood tests assess organ function, electrolyte balance, and signs of infection.
Imaging studies play a crucial role in diagnosis and assessment. Abdominal ultrasound can detect gallstones and inflammation, while CT scans provide detailed images of pancreatic damage and complications. MRI may be used to examine the pancreatic and bile ducts more closely.
Physical examination reveals abdominal tenderness, and in some cases, Grey Turner's sign (bruising around the flanks) or Cullen's sign (bruising around the umbilicus), which indicate severe internal bleeding.
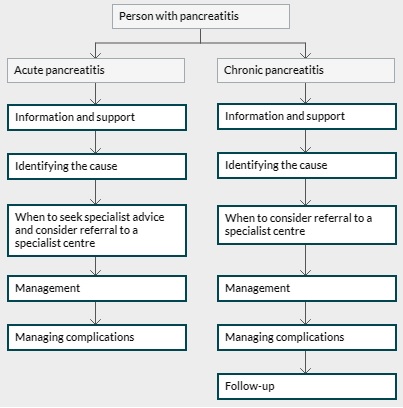
Treatment Approaches for Pancreatitis
Treatment for pancreatitis depends on whether it's acute or chronic and the severity of symptoms. The primary goals are pain management, addressing the underlying cause, and preventing complications.
For acute pancreatitis, initial treatment often requires hospitalization. Patients typically receive:
- Intravenous fluids to prevent dehydration and support organ function
- Pain management through medications, as the pain can be severe
- Fasting to rest the pancreas and prevent further enzyme production
- Nutritional support once inflammation begins to improve
Chronic pancreatitis management focuses on pain control, enzyme replacement therapy, and lifestyle modifications. Patients may need to take pancreatic enzyme supplements with meals to aid digestion and absorb nutrients properly.
Lifestyle Modifications for Prevention
Since alcohol and gallstones are major causes of pancreatitis, lifestyle changes can significantly reduce risk. Consider these preventive strategies:
Limiting alcohol consumption or abstaining entirely if you've experienced pancreatitis before. Even moderate alcohol use can trigger another episode in susceptible individuals.
Maintaining a healthy weight through balanced nutrition and regular exercise helps prevent gallstone formation. A diet rich in fruits, vegetables, whole grains, and lean proteins supports overall pancreatic health.
Avoiding smoking, which increases the risk of both pancreatitis and pancreatic cancer. Studies show that smokers have a 1.5 to 2 times higher risk of developing chronic pancreatitis compared to non-smokers.
Living with Chronic Pancreatitis
For those diagnosed with chronic pancreatitis, daily life requires ongoing management and adaptation. The condition can significantly impact quality of life due to persistent pain, digestive issues, and nutritional challenges.
Dietary modifications become essential, often involving smaller, more frequent meals that are low in fat but rich in nutrients. Working with a registered dietitian can help develop meal plans that minimize pancreatic stimulation while ensuring adequate nutrition.
Pain management may require a combination of medications, including enzyme supplements, pain relievers, and sometimes nerve blocks or other interventional procedures for severe cases.
Emotional support is equally important, as chronic pain and dietary restrictions can lead to anxiety, depression, and social isolation. Support groups and counseling can provide valuable coping strategies.
When to Seek Emergency Care
Understanding when pancreatitis symptoms require immediate medical attention can be life-saving. Seek emergency care if you experience:
- Severe, persistent abdominal pain that doesn't improve with over-the-counter medications
- Pain accompanied by fever, persistent vomiting, or signs of dehydration
- Jaundice (yellowing of skin or eyes), which may indicate bile duct obstruction
- Rapid heartbeat, low blood pressure, or signs of shock
Early intervention can prevent serious complications such as pancreatic necrosis, infection, or organ failure.
The Road to Recovery
Recovery from pancreatitis varies significantly depending on severity and whether it's acute or chronic. Most people with mild acute pancreatitis recover within a week with appropriate treatment, though complete healing may take several weeks.
Prevention of future episodes becomes a priority after the first occurrence. This often involves identifying and addressing underlying causes, whether that means gallbladder removal for gallstone-related pancreatitis or alcohol cessation programs for alcohol-induced cases.
For chronic pancreatitis patients, the focus shifts to managing symptoms and preventing progression. With proper care, many people maintain good quality of life despite the chronic nature of their condition.
Conclusion
Understanding "i get smashed pancreatitis" means recognizing the severe, debilitating pain that characterizes this serious inflammatory condition of the pancreas. Whether acute or chronic, pancreatitis requires prompt medical attention and often involves significant lifestyle modifications for management and prevention.
By recognizing the symptoms, understanding risk factors, and seeking appropriate care, patients can better navigate this challenging condition. Remember that while the pain may feel overwhelming, effective treatments and support systems exist to help manage pancreatitis and improve quality of life.
If you experience severe abdominal pain or suspect you might have pancreatitis, don't hesitate to seek medical care. Early intervention not only provides relief from the "smashed" feeling but also prevents potentially serious complications that could arise from untreated pancreatic inflammation.