What Does A Cavity Look Like When It First Starts? Your Visual Guide To Early Tooth Decay
Have you ever leaned into the mirror, squinting at a suspicious spot on your tooth, and wondered, "What does a cavity look like when it first starts?" You're not alone. This quiet, creeping concern is one of the most common dental questions people have, yet the answer is often shrouded in mystery. Unlike a dramatic, painful break, the earliest signs of a cavity are subtle, silent, and easily missed. Understanding these initial visual cues is your first and most powerful line of defense against progressive tooth decay. This guide will pull back the curtain on the nascent stages of cavities, translating complex dental science into clear, actionable visual knowledge. We'll explore exactly what to look for, why it happens, and what you can do about it before a small spot becomes a major problem.
The journey of a cavity begins not with a hole, but with a chemical siege. Your mouth is a dynamic ecosystem where acids, produced by bacteria feeding on sugars, constantly battle the minerals in your tooth enamel. This first stage, called demineralization, is invisible to the naked eye but is the critical moment where intervention can reverse the process. Think of it like a tiny pothole forming on a road surface; the structure is weakened but not yet collapsed. The key identifier at this microscopic level is a loss of minerals like calcium and phosphate from the enamel crystals. This creates porous, weaker areas that, if unchecked, will manifest as the first visible clues we can actually see.
The Science of the Start: Demineralization and the First Visible Clue
Before we dive into what you can spot, it's essential to understand the how. The process starts with plaque—that sticky, colorless film of bacteria that constantly forms on teeth. When you consume carbohydrates (sugars and starches), these bacteria feast and produce acids as a byproduct. These acids lower the pH in your mouth, creating an acidic environment that leaches minerals out of your enamel's crystalline structure. This is demineralization.
- Ross Dellenger
- Leaked Tianastummys Nude Video Exposes Shocking Secret
- Gary Lockwoods Sex Scandal Leak How It Destroyed His Life
Your body has a natural repair system called remineralization. Saliva, which is rich in calcium and phosphate, along with fluoride from toothpaste or water, helps to replenish these lost minerals and harden the enamel again. A cavity forms when the balance tips too far toward demineralization and the acid attacks are too frequent or prolonged for saliva to keep up. The very first visible sign that this balance has been lost is not a brown hole, but a white spot lesion.
The White Spot Lesion: The #1 Early Visual Indicator
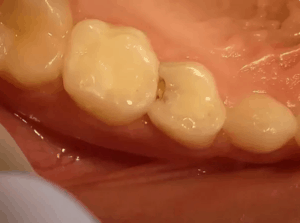
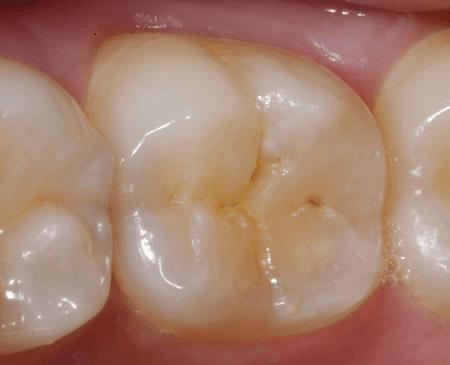
This is the answer to your question in its purest form. A white spot lesion appears as a small, opaque, chalky-white area on the tooth surface. It's most commonly found in the grooves and pits of molars (your back chewing teeth) or along the gumline, but can appear anywhere enamel is present. What you are seeing is a section of enamel that has become porous and less dense due to mineral loss. The way light scatters through this porous area differs from the healthy, dense, translucent enamel surrounding it, creating that distinctive matte, white appearance.
- Where to Look: Pay closest attention to the occlusal surfaces (chewing tops) of your molars and premolars, especially in the deep fissures. Also inspect the buccal surfaces (the cheek-side) of your upper front teeth near the gumline, a common spot for early decay due to plaque accumulation.
- Texture Check: Run your tongue or a clean fingernail gently over the area. A white spot lesion often feels slightly rougher or less smooth than the surrounding enamel, though it's not yet a physical hole.
- It's Not Always a Cavity: Crucially, a white spot can sometimes indicate fluorosis (excess fluoride intake during tooth development) or enamel hypoplasia (a defect in enamel formation). However, in an adult, a new or changing white spot is a major red flag for active, early decay.
Beyond the White Spot: Other Subtle Early Signs
While the white spot is the hallmark, other early changes can occur, often in conjunction with it. These signs are even more easily overlooked but are part of the same destructive process.
- Eva Violet Nude
- Shocking Leak Canelos Secret Plan To End Crawfords Career You Wont Believe This
- Al Pacino Young
Discoloration and Opacity Changes
As demineralization progresses, the enamel's structure continues to degrade. The initial bright white spot may begin to darken slightly, turning into a more yellow, brown, or grayish hue. This happens because the porous enamel allows the underlying, naturally yellower dentin (the layer beneath enamel) to show through more prominently. The lesion may also become more defined, with sharper borders separating it from healthy enamel. You might notice a small area that looks "stained" but doesn't brush away. This is a classic sign that decay is advancing beneath the surface.
The "Shadow" Effect
Sometimes, especially with decay between teeth (interproximal decay), you won't see a distinct spot on the tooth surface. Instead, you might notice a dark shadow or line when you look at the tooth from the side or in a mirror. This shadow is light being absorbed by the demineralized, porous enamel and the underlying dentin. It's a warning that decay has penetrated the enamel and is approaching or has reached the dentin, which is much softer and less resistant to acid.
Sensitivity: The Body's Whisper
Early decay doesn't always hurt, but it can send subtle signals. You might experience a brief, sharp zing when consuming something very cold, hot, or sweet. This transient sensitivity occurs because the porous, weakened enamel allows stimuli to reach the nerve endings in the dentin more easily. The key word is transient—the pain should subside quickly once the stimulus is removed. Persistent, throbbing pain indicates the decay has likely reached the pulp (nerve) and is no longer in the "first start" phase.
How to Detect Early Cavities: Your At-Home and Professional Toolkit
Detecting these early signs requires a combination of vigilant self-examination and professional dental expertise.
Your Daily Inspection Routine
- Good Lighting: Examine your teeth in bright, natural light after brushing and drying them.
- Use a Mirror: A small, handheld dental mirror (available at drugstores) can help you see the tops and backs of molars.
- Look for Changes: Don't just look for spots; look for changes. Is there a new line, a new area of opacity, or a spot that seems different from last month?
- Feel with Your Tongue: Your tongue is a surprisingly sensitive detector. Run it over all surfaces. Note any areas that feel rough, sticky, or "gritty" compared to the smooth feel of your other teeth.
The Dentist's Superior Tools: Why Check-Ups Are Non-Negotiable
Your at-home exam is helpful, but it's no substitute for a professional. Dentists use tools and techniques that reveal what the naked eye cannot:
- Explorer (Dental Probe): A sharp, slender instrument used to gently feel for softness, stickiness, or catch in the enamel. A healthy surface is hard and smooth; an early carious lesion may feel slightly soft or the explorer will "catch" in a pit or fissure.
- X-Rays (Bitewings): This is the gold standard for detecting interproximal decay (between teeth), which is often invisible until it's large. X-rays show dark shadows where mineral density has been lost. They can detect decay when it's still confined to the enamel, long before a hole forms.
- DIAGNOdent Laser: Some dentists use this advanced tool, which emits a laser that measures the fluorescence of tooth structure. Decayed areas fluoresce differently than healthy enamel, providing a numerical reading of decay severity.
Prevention and Reversal: Your Action Plan for Early Decay
The fantastic news about the earliest stage of a cavity (the white spot lesion) is that it can often be reversed. The process of remineralization can rebuild the enamel if you intervene decisively.
1. Optimize Your Oral Hygiene
- Fluoride is Your Best Friend: Use a fluoride toothpaste and consider a fluoride mouthwash. Fluoride attracts minerals, accelerates remineralization, and makes enamel more acid-resistant.
- Master Your Technique: Brush for two full minutes, twice a day, with a soft-bristled brush. Angle the bristles at a 45-degree angle to the gumline to disrupt plaque in the critical sulcus area. Don't forget your tongue!
- Floss Relentlessly: Floss or use interdental brushes daily to remove plaque from between teeth, where 40% of tooth surfaces are missed by brushing alone. This is critical for preventing interproximal white spots.
2. Smart Dietary Choices
- Limit Snacking & Sipping: Every time you eat or drink something sugary/acidic, your mouth's pH drops and stays acidic for 20-30 minutes. Constant grazing prevents your mouth from returning to a neutral, remineralizing state.
- Choose Tooth-Friendly Foods: Cheese, plain yogurt, and fibrous vegetables stimulate saliva and can help neutralize acids. Drink plenty of water, especially fluoridated water.
- Rinse After Acids: If you do consume acidic drinks (soda, juice, sports drinks), don't brush immediately. Rinse with water and wait at least 30 minutes for saliva to begin remineralizing the softened enamel.
3. Professional Interventions for Early Lesions
If your dentist spots an early white spot lesion, they have several non-invasive options:
- Topical Fluoride or CPP-ACP: A high-concentration fluoride varnish or a product like GC Tooth Mousse (containing casein phosphopeptide-amorphous calcium phosphate) can be applied in-office. These deliver a massive dose of remineralizing minerals directly to the lesion.
- Sealants: For pits and fissures on molars, a thin plastic resin sealant can be painted into the grooves, creating a smooth, plaque-resistant barrier that prevents decay from starting in these vulnerable nooks.
- Microabrasion: For superficial white spots, a dentist can use a gentle abrasive and acid to remove a tiny amount of enamel, often eliminating the discoloration entirely.
Frequently Asked Questions About Early Cavities
Q: Can a cavity heal on its own without a filling?
A: Yes, but only at the very earliest stage—the white spot lesion. Once a physical hole (cavity) has formed in the enamel, the structure is lost and cannot regenerate. That hole will need a filling. The goal is to catch and reverse it before the hole forms.
Q: Are cavities always brown or black?
A: No. The classic "cavity" we imagine is a late-stage, advanced lesion. The first visual sign is almost always a white spot. Brown or black discoloration indicates the decay has progressed deeper into the dentin.
Q: Do all white spots mean I have a cavity?
A: Not necessarily. As mentioned, they can be from fluorosis or enamel defects. However, in an adult with a previously normal-appearing tooth, a new white spot is highly likely to be early decay until proven otherwise by a dentist.
Q: Why do I get cavities even though I brush?
A: Brushing is just one part. Cavities are caused by a combination of factors: susceptible teeth (enamel strength), acid-producing bacteria, and a diet that fuels those bacteria (sugars/starches). You must address all three: strengthen enamel (fluoride), reduce bacteria (effective hygiene), and starve bacteria (diet).
Q: How long does it take for a cavity to form?
A: There's no set timeline. It depends on your individual oral chemistry, diet, hygiene, and even saliva flow. The process from initial demineralization to a visible white spot can take months or even years of constant acid attack. This is why consistent daily habits are so critical—you're playing a long-term game of prevention.
Conclusion: Become the Guardian of Your Own Smile
So, what does a cavity look like when it first starts? It looks like a tiny, chalky-white shadow on your tooth, a place where the light doesn't quite bounce back the same way. It might feel slightly rough to your tongue. It might whisper a fleeting sensitivity to an ice cube. It is the silent, first chapter of a story that, if ignored, will end with drilling, filling, and expense. But armed with this knowledge, you hold the power to edit that ending.
Your daily vigilance—the careful inspection, the disciplined brushing and flossing, the mindful eating—is your primary prevention. Your partnership with your dentist through regular check-ups and cleanings is your early warning system. Remember, the goal isn't just to find cavities early; it's to prevent them from ever forming at all. By understanding that the first sign is a reversible white spot, you transform from a passive observer into an active guardian of your oral health. The next time you peer into the mirror, look not with anxiety, but with informed confidence. You now know exactly what to look for, and more importantly, you know precisely what to do about it.