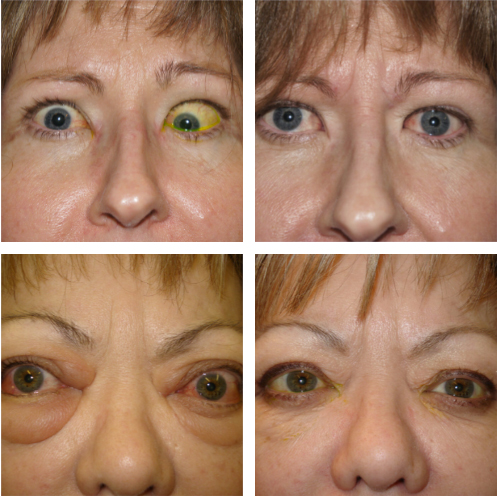
Graves Disease Eyes Photos: What They Reveal About Thyroid Eye Disease
Have you ever typed “Graves disease eyes photos” into a search engine? That simple query opens a window into a complex medical condition affecting thousands, revealing more than just images—it tells a story of autoimmune activity, visible transformation, and the critical importance of early detection. For patients newly diagnosed with Graves’ disease, for family members seeking to understand a loved one’s changing appearance, or for medical students learning the nuances of endocrine disorders, these photographs serve as a powerful educational tool. They capture the tangible reality of an internal battle, showcasing the spectrum of thyroid eye disease (TED), also known as Graves’ ophthalmopathy (GO). This article delves deep into the world of Graves disease eyes photos, explaining what they show, why they matter, how the condition progresses, and what can be done about it. We’ll move beyond the surface to understand the medical science, the patient experience, and the role of visual documentation in managing this challenging aspect of an autoimmune disorder.
Understanding Graves’ Ophthalmopathy: More Than Just “Bulging Eyes”
Before interpreting any photograph, it’s essential to understand the condition itself. Graves’ ophthalmopathy is an inflammatory autoimmune disorder where the body’s immune system mistakenly attacks the tissues around the eyes. This attack targets the extraocular muscles (the muscles that move the eyes) and the orbital fat (the soft tissue padding within the bony eye socket). The culprit is often the same autoimmune process that causes Graves’ disease, an overactive thyroid (hyperthyroidism), but TED can occur even when thyroid function is normal or under control.
The inflammation leads to a cascade of events: swelling, buildup of glycosaminoglycans (GAGs) like hyaluronic acid, and eventually, the deposition of fibrous scar tissue. Because the eye socket is a confined, bony space, this swelling has nowhere to go. The result is a forward displacement of the eyeball (proptosis or exophthalmos), increased pressure behind the eye, and a host of other symptoms. It’s crucial to dispel the myth that TED is merely about “bulging eyes.” While proptosis is a hallmark sign, the condition encompasses a wide range of presentations, from mild redness and irritation to severe, sight-threatening complications. Graves disease eyes photos often capture this full spectrum, making them invaluable for awareness and diagnosis.
The Autoimmune Link: Why the Eyes?
The connection between the thyroid and the eyes lies in a shared antigen. The thyroid-stimulating hormone receptor (TSHR) is found not only on thyroid cells but also on fibroblasts within the orbital tissues. In Graves’ disease, the immune system produces thyroid-stimulating immunoglobulins (TSIs) that bind to and activate these receptors. In the orbit, this activation prompts fibroblasts to transform into fat cells (adipogenesis) and produce inflammatory substances and GAGs. This orbital-specific inflammation is what leads to the distinctive eye changes. Smoking is the single most significant environmental risk factor, dramatically increasing both the likelihood of developing TED and its severity.
Decoding the Visuals: A Symptom-by-Symptom Guide to Graves Disease Eyes Photos
When you look at a series of Graves disease eyes photos, you are witnessing the physical manifestations of orbital inflammation. Understanding what each visual cue means transforms a simple image into a diagnostic narrative. Let’s break down the key features you might observe.
The Classic Stare: Proptosis and Exophthalmos
The most recognized feature is proptosis—the abnormal protrusion of the eyeball from the orbit. This gives the characteristic “staring” or “frightened” appearance. The degree of proptosis is measured in millimeters from the corneal apex to a line connecting the frontal bones (the exophthalmometer reading). Photos clearly show the increased scleral show (the white of the eye above or below the iris), the stretching of the eyelids, and the potential for lagophthalmos (inability to close the eyelids completely). It’s important to note that proptosis can be asymmetric, affecting one eye more than the other, which is frequently visible in comparative photos.
- Sky Bri Leak
- Jaylietori Nude
- Shocking Leak Canelos Secret Plan To End Crawfords Career You Wont Believe This
The Red, Irritated Gaze: Conjunctival and Eyelid Changes
Inflammation is rarely subtle. Graves disease eyes photos often highlight:
- Conjunctival redness (chemosis): The clear membrane covering the white of the eye becomes swollen and red, resembling a “wet” or “watery” appearance.
- Periorbital edema: Puffiness and swelling of the eyelids and the soft tissues around the eye socket.
- Eyelid retraction: The upper eyelid is pulled upward, and sometimes the lower lid is pulled down, exposing more of the eyeball. This is caused by inflammation and fibrosis of the levator muscle (which lifts the upper lid) and Müller’s muscle. This retraction contributes significantly to the staring look.
- Lid lag: On downward gaze, the upper eyelid fails to follow the cornea smoothly, remaining higher than normal.
The Gaze That Strays: Strabismus and Diplopia
Inflammation and subsequent scarring of the extraocular muscles restrict eye movement. This leads to strabismus (misalignment of the eyes) and diplopia (double vision). In photos, this may manifest as one eye appearing slightly turned inward, outward, up, or down. Patients often report that double vision is worse when looking in the direction of the affected muscle. Advanced photos might show a noticeable head tilt, a compensatory mechanism the patient adopts to align the eyes and reduce double vision.
The Pressure Build-Up: Optic Nerve Compression
This is the most serious complication. Swelling in the confined orbital space can compress the optic nerve, which carries visual signals from the eye to the brain. Graves disease eyes photos cannot show this directly, but they may capture signs suggestive of it: a pale or swollen optic disc (seen only during an eye exam), or more subtly, a patient with significant proptosis and complaints of blurred vision, loss of color vision, or visual field defects. This is a medical emergency requiring immediate treatment to prevent permanent vision loss.
The Skin’s Story: Pretibial Myxedema and Acropachy
While not on the eyes, these are related extrathyroidal manifestations. Pretibial myxedema is thick, reddened, peau d’orange (orange peel) skin on the shins, present in about 1-3% of TED patients. Digital clubbing (acropachy) involves swollen fingertips and nail changes. Including these in a patient’s photographic record provides a complete picture of their autoimmune activity.
The Clinical Camera: Why Doctors Document Graves Disease Eyes Photos
Medical photography is a cornerstone of managing Graves’ ophthalmopathy. It is not for sensationalism but for precise, objective care. Graves disease eyes photos serve several critical clinical functions:
- Baseline Documentation: At diagnosis, standardized photos (front, side, upward, downward gaze) establish a visual baseline. This is crucial for tracking progression or improvement over time.
- Objective Measurement: They allow for accurate measurement of proptosis (using Hertel exophthalmometer readings alongside the photo), eyelid retraction, and strabismus angles, reducing reliance on subjective memory.
- Monitoring Response to Treatment: Comparing “before and after” photos after treatments like corticosteroids, radiation, or surgery provides undeniable evidence of efficacy for both doctor and patient.
- Patient Education and Empowerment: Showing patients their own photos helps them understand the severity of their condition, the rationale for treatment recommendations, and the tangible results of interventions.
- Multidisciplinary Communication: These photos facilitate clear communication between endocrinologists, ophthalmologists, and orbital surgeons, ensuring all specialists are on the same page.
The Art of Standardized Photography
For clinical photos to be useful, they must be consistent. This means:
- Fixed Distance and Angle: Using a tripod at a set distance.
- Standardized Gaze: Photos in primary position (looking straight ahead), upgaze, and downgaze.
- Neutral Expression: No smiling or squinting.
- Lighting: Consistent, shadow-free lighting.
- Scale: A ruler or known-size object in the frame for scale, especially in research settings.
The Patient’s Lens: The Psychological Impact and The Search for “Graves Disease Eyes Photos”
The decision to search for “Graves disease eyes photos” is often fraught with emotion. For a patient recently noticing changes in the mirror, this search is a quest for validation, understanding, and community. Seeing images that mirror their own experience can be both frightening and relieving—frightening because it confirms a serious diagnosis, but relieving because it ends the isolation of wondering “what is wrong with me?”
This visual journey taps into profound psychological impacts:
- Altered Self-Image and Identity: The face is central to identity. Sudden, visible changes can lead to grief, anxiety, depression, and social withdrawal.
- Staring and Unsolicited Comments: Patients often report being stared at or asked about their eyes, which can be deeply distressing.
- Quality of Life: Studies using validated questionnaires like the Graves’ Ophthalmopathy Quality of Life (GO-QOL) score show that TED significantly impacts daily functioning, emotional well-being, and social interactions, often more than the underlying thyroid disease itself.
Finding accurate, representative photos online is a double-edged sword. While it provides information, it can also trigger anxiety. Patients must be cautious, ensuring sources are reputable (medical institutions, patient advocacy groups like the Graves’ Disease & Thyroid Foundation) to avoid misinterpreting extreme cases as the only possibility.
Treatment Pathways: From Medication to Surgery – What Photos Can’t Show
While photos document the “what,” treatment addresses the “why” and “how.” Management is tailored to disease activity and severity. Graves disease eyes photos show the result, but not the complex decision-making behind the treatment.
Phase 1: Active, Inflammatory Disease
The goal is to suppress inflammation and halt progression.
- Systemic Corticosteroids: High-dose oral or intravenous (IV) steroids (e.g., methylprednisolone) are first-line to reduce acute inflammation and swelling. IV pulses are often preferred for better efficacy and fewer long-term side effects.
- Orbital Radiotherapy: Low-dose radiation to the orbits can reduce inflammation, particularly helpful for diplopia and soft tissue swelling, often used in combination with steroids.
- Newer Targeted Therapies:Teprotumumab (Tepezza®), a monoclonal antibody that blocks the IGF-1 receptor, has revolutionized treatment for active, moderate-to-severe TED, showing dramatic reductions in proptosis and inflammation in clinical trials. Rituximab is used off-label in some refractory cases.
- Selenium: For mild active disease, selenium supplements (200mcg/day) have been shown to improve quality of life and slow progression in some studies.
- Supportive Care: This is vital for all patients and includes:
- Lubricating Eye Drops/Gels: To combat exposure from lagophthalmos.
- Prism Glasses: For temporary relief of diplopia.
- Head Elevation: To reduce overnight fluid accumulation and swelling.
- Strict Smoking Cessation: The single most important modifiable factor.
Phase 2: Inactive, “Burnt-Out” Disease
Once inflammation subsides (usually after 6-18 months), the focus shifts to correcting residual deformities.
- Orbital Decompression Surgery: The bony walls of the orbit are removed or thinned to create more space, allowing the swollen tissues to fall back into the skull. This reduces proptosis, relieves optic nerve compression, and can improve eyelid retraction. It is often the most transformative procedure visible in “after” Graves disease eyes photos.
- Strabismus Surgery: To realign the eyes and eliminate persistent diplopia.
- Eyelid Surgery (Blepharoplasty): To correct retraction, improve closure, and remove excess skin or fat, creating a more natural appearance.
Navigating the Online World: How to Search for and Interpret Graves Disease Eyes Photos Responsibly
If you are searching for these images, here is a responsible approach:
- Define Your Goal: Are you looking for mild examples? Severe cases? Before-and-after surgery photos? Use specific search terms like “mild Graves ophthalmopathy,” “severe thyroid eye disease proptosis,” or “orbital decompression results.”
- Use Credible Sources: Prioritize results from:
- Academic medical centers (e.g., Mayo Clinic, Cleveland Clinic, Johns Hopkins).
- Patient advocacy organizations (Graves’ Disease & Thyroid Foundation, BTF – British Thyroid Foundation).
- Peer-reviewed medical journals (though full articles may require subscription, abstracts and some images are public).
- Understand the Spectrum: Remember, you will see the most dramatic cases online. Mild disease is less likely to be photographed and shared. Do not compare your early-stage symptoms to end-stage, severe photos, as this can cause unnecessary panic.
- Look for Context: Reputable sources will caption images with information about disease stage, activity, and treatments. This context is everything.
- Talk to Your Doctor: Bring screenshots or questions to your appointment. Your doctor can interpret what you see in the context of your specific case.
Frequently Asked Questions About Graves Disease Eyes Photos
Q: Can Graves disease eyes photos predict how my eyes will look?
A: No. While photos show the range of possibilities, your specific outcome depends on a unique combination of disease activity, severity, genetics, smoking status, and response to treatment. Your doctor can give you a prognosis based on your individual exam and tests, not on general photos.
Q: Are there “typical” Graves disease eyes photos?
A: There is a classic presentation (proptosis, lid retraction, redness), but the appearance is highly variable. Some patients have primarily swelling and redness with minimal bulge (inflammatory phenotype), while others have significant forward displacement with less redness (fibrotic phenotype). Photos reflect this diversity.
Q: Should I take my own Graves disease eyes photos?
A: Absolutely! With your doctor’s guidance, taking standardized photos at home (same lighting, distance, gaze) can be an excellent tool for self-monitoring between appointments. It helps you and your doctor notice subtle changes you might otherwise miss.
Q: Do all people with Graves’ disease get eye problems?
A: No. Approximately 25-30% of patients with Graves’ hyperthyroidism will develop clinically obvious ophthalmopathy. However, subclinical changes (detectable only by MRI or specialized exams) are more common. The risk is much higher in smokers.
Q: Can treatment make my eyes look exactly like they did before Graves’?
A: The goal of treatment is to restore function, relieve symptoms, and achieve a natural, symmetric appearance. While modern treatments like teprotumumab and orbital decompression can achieve remarkable improvements, perfect reversal to the pre-disease state is not always possible, especially in long-standing, fibrotic cases. The aim is the best possible outcome for you.
Conclusion: The Image and the Reality Beyond It
The search for “Graves disease eyes photos” is more than a simple image query; it is a gateway to understanding a complex interplay of endocrinology, immunology, and ophthalmology. These photographs are powerful educators, shattering the misconception that this is a trivial cosmetic issue. They reveal a condition that can cause physical discomfort, threaten sight, and devastate self-esteem. Yet, within the frames of these images, we also see the profound success of modern medicine—the restored symmetry after surgery, the relieved pressure after effective medical therapy, the return of a natural gaze.
If you are looking at these photos because you suspect changes in your own eyes, let them be a catalyst for action, not fear. Schedule an evaluation with an ophthalmologist specializing in orbital disease and an endocrinologist. If you are a caregiver or student, let these images foster empathy and a deeper scientific curiosity. The story told by Graves disease eyes photos is ultimately one of resilience—the resilience of the human body under autoimmune siege and the resilience of patients and physicians working together to reclaim health and appearance. The next time you encounter such an image, look beyond the surface. See the inflammation, the pressure, the struggle—and then see the hope, the treatment pathways, and the possibility of a clearer, brighter future.