Melanoma On The Scalp: The Hidden Danger You Might Be Overlooking
Have you ever carefully examined your scalp for signs of skin cancer? For most people, the answer is no. When we think about skin checks, our minds typically go to our arms, face, or legs. Yet, one of the most common and dangerously overlooked locations for a potentially deadly form of skin cancer is right on top of our heads: melanoma on the scalp. This stealthy adversary often hides in plain sight, concealed by hair, and is frequently diagnosed at a later, more aggressive stage than melanomas on other parts of the body. Understanding this hidden threat is not just about awareness—it’s a critical component of your long-term health and survival.
The scalp is a unique and high-risk environment for melanoma development. It receives intense, repeated sun exposure throughout our lives, often without the benefit of consistent sunscreen application. Unlike other areas, it’s difficult to self-examine thoroughly, and lesions can grow undetected for months. This combination of factors contributes to a poorer prognosis for scalp melanoma compared to melanomas on the limbs or trunk. But knowledge is power. By learning the risks, recognizing the warning signs, and adopting proactive prevention strategies, you can dramatically improve your chances of early detection and successful treatment. This comprehensive guide will illuminate every critical aspect of melanoma on the scalp, empowering you to protect yourself and your loved ones.
Understanding Melanoma: More Than Just a "Mole"
Before diving into the specifics of the scalp, it’s essential to understand what melanoma is. Melanoma is a type of skin cancer that originates in the melanocytes, the cells responsible for producing melanin, the pigment that gives skin its color. While it is less common than other skin cancers like basal cell carcinoma or squamous cell carcinoma, melanoma is by far the most dangerous. It has a high propensity to spread (metastasize) to other parts of the body if not caught early.
- The Secret Sex Tape Everyones Talking About Michelle Myletts Leaked Scandal Exposed
- The Nude Truth About Room Dividers How Theyre Spicing Up Sex Lives Overnight
- Bernice Burgos Shocking Leaked Video Exposes Everything
Melanoma can develop from an existing mole or appear as a new, unusual growth on the skin. It is primarily caused by intense, intermittent UV radiation exposure (like sunburns), especially in childhood and adolescence, though cumulative sun exposure over a lifetime also plays a significant role. Genetic factors can also increase risk. The key takeaway is that any new, changing, or unusual skin lesion warrants professional evaluation. When this occurs on the scalp, the stakes are uniquely high due to the area's anatomy and the challenges of detection.
Why the Scalp is a High-Risk Zone for Melanoma
The scalp is not just another patch of skin; it presents a perfect storm of risk factors that make it a particularly concerning site for melanoma development.
The Sun Exposure Factor
The scalp is almost always exposed to the sun. For men with thinning hair or baldness, and for anyone who spends significant time outdoors without a hat, the scalp receives direct, unfiltered UV radiation. Even with a full head of hair, parts can thin over time, creating vulnerable zones. The scalp's skin is also often thinner than on other body parts, potentially allowing UV damage to penetrate more deeply. This chronic, high-dose exposure is a primary driver for DNA damage in melanocytes, setting the stage for cancer.
- The Untold Story Of Mai Yoneyamas Sex Scandal Leaked Evidence Surfaces
- Exposed Janine Lindemulders Hidden Sex Tape Leak What They Dont Want You To See
- 3 Jane Does Secret Life The Hidden Story That Will Change Everything You Thought You Knew
The Detection Dilemma
This is perhaps the most critical issue. Hair acts as the ultimate camouflage. A growing melanoma can be completely hidden from view. People rarely part their hair systematically to inspect their scalp. By the time a lesion becomes visible at the hairline, causes bleeding, or is felt as a lump, it may have been growing for many months or even years. This delay in detection is a major reason why scalp melanomas are, on average, thicker and more advanced at diagnosis than melanomas on more visible areas.
Biological and Anatomical Considerations
The scalp has a rich blood supply and is connected to a dense network of lymph vessels. This provides a potential superhighway for cancer cells to metastasize to distant organs more quickly compared to a melanoma on, say, the forearm. Furthermore, the skin on the scalp is tightly adherent to the underlying galea aponeurotica and skull, meaning a tumor can invade these structures more readily than on more mobile skin.
Demographic Risk Factors
Certain populations are at higher risk for scalp melanoma. Men over 50 with pattern baldness (androgenetic alopecia) are at the highest risk, likely due to the combination of chronic sun exposure on a thinning scalp and potential delays in detection. Older adults in general are at higher risk simply due to cumulative sun damage over decades. Individuals with a personal or family history of melanoma, numerous atypical moles, or fair skin that burns easily are also at increased risk for scalp involvement.
Recognizing the Signs: What to Look For on Your Scalp
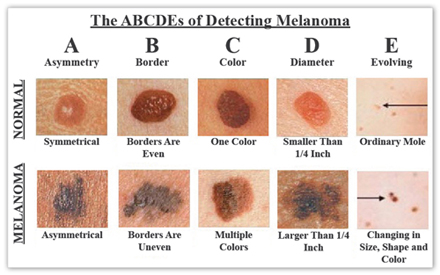
The principles for spotting melanoma on the scalp are the same as for any part of the body, famously summarized by the ABCDE rule. However, applying this rule to the scalp requires a bit more effort and a systematic approach.
The ABCDE Rule for Scalp Lesions
- A - Asymmetry: One half of the mole or lesion does not match the other half. If you could draw a line through the middle, the two sides would look different.
- B - Border: The edges are irregular, scalloped, or poorly defined. They may look blurry, notched, or ragged, rather than smooth and even.
- C - Color: The color is not uniform. Look for shades of tan, brown, black, but also patches of red, white, blue, or gray. A melanoma can have multiple colors within one lesion.
- D - Diameter: The diameter is typically larger than 6mm (about the size of a pencil eraser). However, any diameter is concerning if the lesion shows other ABCDE features or is changing. Scalp melanomas can be smaller.
- E - Evolving: This is the most crucial sign. The mole or lesion is changing in size, shape, color, elevation, or new symptoms like itching, tenderness, or bleeding. Any evolution warrants immediate medical attention.
Additional "Ugly Duckling" Signs
Sometimes, a melanoma doesn't fit the ABCDE mold perfectly. The "ugly duckling" sign is a powerful concept: a mole that looks different from all your other moles. If one spot on your scalp stands out as being a different color, shape, or texture from your other nevi, it’s a red flag.
Specific Scalp Symptoms to Heed
Because the scalp is hairy and sensitive, symptoms can be mistaken for other issues like dandruff, psoriasis, or a minor scratch. Be alert for:
- A new, persistent pimple, sore, or scab that doesn't heal within a few weeks.
- A spot that bleeds easily with minor rubbing (like from brushing hair).
- A raised, firm nodule or bump, which may be skin-colored, pink, red, or dark.
- Persistent itching, tenderness, or pain in a specific, localized area.
- A mole that has become raised from a previously flat spot.
- Hair loss in a very small, circular patch directly over a lesion (a less common but possible sign).
The Critical Importance of Professional Diagnosis
You cannot diagnose melanoma by sight or feel alone. A suspicious lesion on the scalp requires evaluation by a board-certified dermatologist. The gold standard for diagnosis is a skin biopsy.
The Biopsy Process
During a biopsy, the dermatologist will numb the area and remove all or part of the suspicious lesion. There are several types:
- Excisional Biopsy: The preferred method for suspected melanoma. The entire lesion, with a small margin of surrounding normal skin, is removed down to the subcutaneous fat. This allows the pathologist to see the full architecture of the tumor and measure its thickness (Breslow thickness), the single most important prognostic factor.
- Incisional Biopsy: If the lesion is very large, a representative sample may be taken.
- Punch Biopsy: A small, circular tool removes a core sample. It can be used but may not capture the deepest part of a thick lesion, so its use on the scalp must be carefully considered.
The removed tissue is sent to a dermatopathologist who examines it under a microscope to confirm if cancer cells are present and, if so, determines the specific type, depth, and other characteristics that guide treatment.
Staging and Further Testing
If melanoma is confirmed, staging determines how far it has spread. This may involve:
- Sentinel Lymph Node Biopsy (SLNB): A procedure to check if cancer cells have reached the nearest lymph nodes (often in the neck or behind the ear for scalp melanomas). A radioactive tracer and/or dye is injected near the tumor site to identify the "sentinel" node(s), which are then removed and examined.
- Imaging: For thicker melanomas or those with symptoms suggesting spread, CT, MRI, or PET scans may be used to check distant organs like the lungs, liver, or brain.
Treatment Pathways for Scalp Melanoma
Treatment is highly personalized based on the stage of the cancer.
Surgical Excision: The Cornerstone
For early-stage (Stage 0, I, II) melanoma, the primary treatment is surgical excision with wider margins than the initial diagnostic biopsy. The margin width depends on the Breslow thickness. For a 1mm thick melanoma, a 1-2cm margin of normal-appearing skin is typically removed. On the scalp, this can sometimes require complex closure techniques or skin grafts, especially for larger defects. The goal is to remove all cancer cells with a clean border.
Management of Advanced Disease
For Stage III (spread to lymph nodes) or Stage IV (distant metastasis), treatment becomes systemic.
- Immunotherapy: Drugs like pembrolizumab (Keytruda) or nivolumab (Opdivo) help the patient's own immune system recognize and attack cancer cells. They have revolutionized the prognosis for advanced melanoma.
- Targeted Therapy: For melanomas with a specific BRAF gene mutation (present in about half of cases), drugs like dabrafenib and trametinib target that mutation to slow or stop cancer growth.
- Radiation Therapy: May be used after lymph node removal to reduce recurrence risk in the nodal basin, or to treat specific metastatic sites, such as brain metastases.
- Chemotherapy: Used less frequently now, but may be an option in certain situations.
The treatment plan is developed by a multidisciplinary team including surgical oncologists, medical oncologists, radiation oncologists, and dermatologists.
Prevention and Early Detection: Your Action Plan
Since early detection is so crucial for scalp melanoma, a proactive approach is non-negotiable.
Sun Protection is Non-Negotiable
- Wear a Wide-Brimmed Hat: This is the single most effective physical barrier for your scalp, face, and neck. Choose a hat with at least a 3-inch brim all around.
- Use Scalp-Specific Sunscreen: Spray-on or stick sunscreens designed for the scalp/hairline are less messy and easier to apply. Look for broad-spectrum SPF 30 or higher. Reapply every two hours and after swimming or sweating.
- Seek Shade: Especially between 10 a.m. and 4 p.m., when UV rays are strongest.
- Avoid Tanning Beds: They emit intense UV radiation and are a known carcinogen.
Master the Scalp Self-Exam
You must become familiar with the landscape of your own scalp. Here’s how:
- Use a Full-Length Mirror and a Handheld Mirror: In a well-lit room, part your hair in small sections using a comb or your fingers. Start at the front hairline and work your way systematically to the crown and nape of the neck.
- Ask for Help: Enlist a partner, family member, or friend. They can see areas you cannot, like the very top and back of your head. Teach them what to look for using the ABCDE rule.
- Feel Your Scalp: Run your fingertips over your entire scalp. Feel for any new lumps, bumps, or rough patches that weren't there before.
- Take Photos: If you have many moles or a concerning spot, take clear, well-lit photos with a ruler for scale. This helps you track any changes over time.
- Frequency: Perform a thorough self-exam monthly. Schedule a professional full-body skin exam with a dermatologist annually, or more frequently if you have a personal or strong family history of skin cancer.
Know Your Risk
Be honest with yourself about your risk factors: fair skin, history of sunburns, numerous moles, family history, immunosuppression. If you are high-risk, discuss a more frequent screening schedule with your dermatologist.
Living With and Beyond Scalp Melanoma
A diagnosis of melanoma is life-changing, but not a guaranteed death sentence, especially with early detection. For those who have had melanoma, vigilance is a lifelong commitment.
The Risk of Recurrence
People who have had melanoma are at higher risk for developing a second melanoma. This makes rigorous, lifelong surveillance essential. This includes:
- Religiously following the self-exam and professional exam schedule.
- Meticulous sun protection for life.
- Being aware that melanomas can occur in unusual locations, including the scalp, even after a melanoma on another body part has been treated.
The Emotional and Practical Impact
Treatment for scalp melanoma, especially surgery, can result in scarring and hair loss. This can have a significant psychological impact. Discuss reconstruction options with your surgical team. Support groups, both in-person and online, can provide invaluable emotional support and practical advice from others who have walked a similar path.
Conclusion: Your Scalp Deserves a Second Look
Melanoma on the scalp is a formidable opponent, thriving in the shadows cast by our own hair. Its tendency for late diagnosis and aggressive behavior makes it a silent killer we can no longer afford to ignore. The statistics are sobering: while scalp melanomas represent only 2-5% of all melanomas, they are often thicker at diagnosis and associated with lower survival rates compared to melanomas on the limbs. This disparity is almost entirely due to delayed detection.
The solution is straightforward but requires discipline: awareness, regular examination, and prompt action. Integrate scalp checks into your monthly skin self-exam routine. Invest in a good hat and make scalp sunscreen a habit, just like brushing your teeth. Schedule that annual dermatologist appointment and specifically ask them to examine your scalp thoroughly. If you notice any new, changing, or unusual spot—no matter how small or seemingly insignificant—make an appointment. Do not wait for it to bleed or grow.
Your health is your most valuable asset. Don't let a cancer that is often highly curable in its early stages win because it was hiding in plain sight. Take the time today to part your hair, feel your scalp, and commit to vigilance. The life you save could be your own.