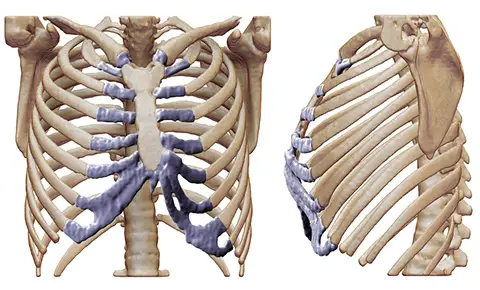
Rib Removal Before And After: Real Results, Risks, And What To Truly Expect
Have you ever found yourself deep in an internet rabbit hole, staring at "rib removal before and after" photos, and wondering what the real story is? Is it a miraculous solution for a sculpted waistline, a necessary medical intervention for chronic pain, or a risky gamble with irreversible consequences? The truth, as with most significant medical procedures, is far more nuanced than the dramatic transformations often depicted online. This comprehensive guide dives deep into the world of rib removal—technically known as costal cartilage resection or rib resection—exploring everything from the surgical realities and recovery journey to the genuine before and after outcomes, both physical and personal. Whether you're exploring this due to a medical condition like thoracic outlet syndrome or considering it for cosmetic refinement, understanding the full spectrum is not just advisable; it's essential for making an informed, safe decision.
A Celebrity Lens: The Curious Case of Cher and Rib Removal Speculation
Before we delve into the clinical and practical details, it's impossible to ignore the pop culture elephant in the room. The topic of rib removal is inextricably linked to speculation about one of Hollywood's most enduring icons: Cher. For decades, rumors have swirled that the singer and actress underwent the procedure to achieve her famously tiny waist, a hallmark of her iconic stage costumes. While Cher has never publicly, definitively confirmed or detailed such a surgery, the persistent gossip and visual comparisons have fueled public fascination and debate about the very possibility of cosmetic rib alteration.
This celebrity case study serves as a powerful, if anecdotal, entry point. It highlights the intense cosmetic motivations that drive some individuals toward this extreme procedure and underscores the importance of separating myth from medical reality. Cher's alleged transformation is often cited in forums and articles discussing "rib removal before and after," making her bio a relevant reference point for understanding the cultural context.
| Personal Detail | Information |
|---|---|
| Full Name | Cherilyn Sarkisian |
| Birth Date | May 20, 1946 |
| Primary Career | Singer, Actress, Television Personality |
| Rumored Procedure | Cosmetic rib removal (speculative, unconfirmed) |
| Notable "Before/After" Era | 1960s (with Sonny Bono) vs. 1970s onward (solo career) |
| Public Stance | Has alluded to extreme dieting and corsetry but not surgical rib removal. |
| Cultural Impact | Her silhouette became a symbol of extreme waist-cinching, directly linking celebrity image to body modification rumors. |
It is critical to note that any discussion of Cher's body is based on public observation and rumor, not on verified medical records. Her case illustrates the potent desire for an aesthetic ideal but should not be taken as a clinical endorsement. The real lessons come from understanding the procedure itself, its legitimate uses, and its profound implications.
What Exactly Is Rib Removal Surgery? Demystifying the Procedure
Rib removal surgery, or costal cartilage resection, is a precise surgical operation where one or more segments of a rib, typically the lower floating ribs (ribs 11 and 12) or portions of the costal cartilage of the upper ribs, are excised. It's not a simple "snip and discard" process. The surgery is performed under general anesthesia by either a thoracic surgeon (for medical cases) or a board-certified plastic surgeon with specific expertise in chest wall surgery (for cosmetic cases). The surgeon makes an incision, often along the natural crease of the lower rib cage or abdomen, carefully separates muscle tissue, and removes the targeted bony or cartilaginous segment. The incision is then closed in layers.
The extent of the removal varies. For medical necessity, such as relieving compression in thoracic outlet syndrome (TOS), the goal is to remove just enough bone or cartilage to decompress nerves and blood vessels. For cosmetic waist sculpting, the aim is to remove a segment of the lower rib cage and/or the overlying cartilage to reduce the protrusion of the "rib flare" and create a smoother, more tapered transition from the torso to the hip. This is often combined with liposuction of the flanks and abdominal etching for comprehensive contouring. The procedure is permanent; once bone or cartilage is removed, it does not regenerate. This permanence is a critical factor in the "before and after" equation, as the changes to the skeletal structure are, for all intents and purposes, irreversible.
Medical Necessity vs. Cosmetic Desire: Two Sides of the Same Coin
Understanding the fundamental distinction between therapeutic and elective rib removal is the cornerstone of this topic. The "before and after" narrative changes dramatically depending on the motivation.
Therapeutic Rib Removal is a legitimate, often life-improving surgery. The most common indication is thoracic outlet syndrome, a condition where nerves or blood vessels between the collarbone and first rib are compressed, causing severe pain, numbness, weakness, and discoloration in the shoulder and arm. When conservative treatments like physical therapy fail, first rib resection (removing the topmost rib) is a well-established surgical solution. According to studies, surgical decompression for neurogenic TOS can lead to significant pain relief and functional improvement in 60-80% of carefully selected patients. Other medical reasons include removing rib tumors (benign or malignant), treating chronic rib infections (osteomyelitis), or repairing severe rib fractures that are not healing properly. The "after" in these cases is measured in pain reduction, restored mobility, and prevention of progressive nerve damage.
Cosmetic Rib Removal, often marketed as "waist sculpting" or "rib flare reduction," is purely elective. It targets individuals, predominantly women, who are genetically predisposed to a wider lower rib cage or pronounced "rib flare" and seek a dramatically smaller waist circumference. The goal is to alter the skeletal framework to achieve an hourglass silhouette that diet and exercise alone cannot. This is an extreme procedure, not a substitute for weight loss. Candidates are typically at a stable, healthy weight but are frustrated by a stubborn bony structure. The "after" here is measured in circumference reduction (often 2-4 inches at the waist) and a change in body proportions. The motivation is aesthetic confidence, not pain relief. This distinction is vital, as it influences everything from insurance coverage (medical is often covered; cosmetic is almost always self-pay) to the ethical considerations of performing irreversible surgery for appearance.
The Surgical Journey: What Happens on the Operating Table
For a patient undergoing either type of rib removal, the "before" state is one of consultation, planning, and pre-operative preparation. The "after" begins in the operating room. The procedure itself typically lasts 2 to 4 hours, depending on complexity. After anesthesia, the surgeon makes the incision. For cosmetic cases targeting the lower ribs, a low transverse incision (similar to a tummy tuck incision) is common, allowing access to the lower rib cage and cartilage. For a first rib resection (TOS), an incision may be made above the clavicle or in the armpit.
The surgeon then meticulously dissects through subcutaneous tissue and muscle (often splitting the latissimus dorsi or serratus anterior muscles to access the ribs). The targeted rib segment is identified, and using specialized bone cutters, a section—usually 1-3 inches long—is removed. In cosmetic cases, the surgeon may also shave or reshape the costal cartilage to smooth the transition. Hemostasis (stopping bleeding) is critical. Once the removal is complete, the muscles are reattached or repositioned, and the incision is closed with sutures or staples. Drainage tubes are often placed to prevent fluid accumulation (seroma or hematoma). The patient awakens in the recovery room with a bandaged torso and likely a patient-controlled analgesia (PCA) pump for pain management. The immediate post-op "after" is marked by significant discomfort, limited mobility, and the beginning of a long healing process.
Recovery and Healing: The Long Road from Surgery to "After"
The romanticized "before and after" photo often skips the grueling recovery phase, which is arguably the most challenging part of the entire journey. The true "after" doesn't begin until months later. Initial recovery in the hospital lasts 1-3 days, focusing on pain control, breathing exercises to prevent pneumonia, and monitoring for complications. Once home, the reality sets in.
- Weeks 1-2: This is the most difficult period. Movement is severely restricted. Patients must avoid twisting, bending, or lifting anything heavier than 5 pounds. Breathing is shallow and painful. Daily activities like showering require assistance. Pain is managed with oral medications. Sleep is often in a recliner to avoid pressure on the incision.
- Weeks 3-6: Gradual improvement. Drainage tubes (if placed) are usually removed within 1-2 weeks. Light walking is encouraged. Many return to a sedentary desk job around 3-4 weeks, but physical exertion remains off-limits. Numbness and tingling around the incision are common.
- Months 2-4: Sutures or staples are removed (if non-dissolvable). More normal activities resume, but contact sports, heavy lifting, and strenuous exercise are still prohibited. The body is still healing internally; the scar tissue is maturing, and the chest wall is stabilizing.
- Months 4-6+: Full recovery. Most patients can return to all normal activities, including intense workouts, around the 4-6 month mark, though some residual stiffness or sensitivity may linger longer. The final "after" result—the settled contour and scar maturation—is not fully visible until 9-12 months post-op.
During this time, adherence to the surgeon's instructions is paramount. This includes wearing any prescribed compression garments, performing prescribed breathing and gentle range-of-motion exercises, and attending all follow-up appointments. Rushing recovery can lead to complications like wound dehiscence (opening), chronic pain, or poor scarring.
Before and After Photos: Interpreting the Visual Evidence
The allure of "rib removal before and after" photos is undeniable. They promise a tangible, visual proof of transformation. However, a critical, skeptical eye is essential when viewing these images, whether from a surgeon's gallery or online forums.
What to Look For in Credible "After" Photos:
- Consistent Angles and Lighting: Professional surgeons use standardized photography protocols. The before and after shots should be taken from the exact same distance, angle, and lighting conditions to ensure a fair comparison.
- Same Pose and Clothing: The subject should be in the same posture (often a relaxed, natural stance with arms slightly away from the body) and wearing similar, form-fitting clothing (like a sports bra and leggings or a bikini top) to accurately assess waist contour.
- Time Stamp: A true "after" result requires patience. Photos taken at 3 months show swelling and healing; the final result at 12+ months shows the settled shape. Surgeons should label the post-op date.
- Full-Body Context: The waist change should be viewed in proportion to the entire silhouette. An unnaturally pinched waist that disrupts natural hip-to-shoulder ratios can be a red flag for over-aggressive surgery.
Common Deceptions to Beware Of:
- Photoshop and Digital Alteration: Unfortunately, many "results" are digitally enhanced. Look for inconsistent backgrounds, shadows, or body proportions.
- The "Suck-It-In" Effect: The "after" photo may be taken with maximal abdominal and core engagement, while the "before" is relaxed. This exaggerates the difference.
- Weight Loss Confounding the Result: Did the patient also lose a significant amount of weight between photos? This would drastically change the waist, making it impossible to attribute the change solely to rib removal.
- Corsetry and Posing: Heavy use of waist-cinching corsets in the "after" photo or strategic posing (twisting the body, specific arm placement) can create an illusion of a smaller waist.
The most honest "before and after" narrative is often told not just in photos, but in the patient's own words about their pain levels, functional improvements, and psychological adjustment.
Risks and Complications: The Unseen Side of the "After"
Every surgical procedure carries risk, but rib removal involves operating on the thoracic cage, which protects vital organs. The potential complications are serious and must be weighed against any perceived benefit.
- Immediate Surgical Risks: Infection, significant bleeding, adverse reaction to anesthesia, and pneumothorax (collapsed lung) are the most dangerous acute risks. A pneumothorax occurs if the lining of the lung (pleura) is inadvertently punctured, allowing air to leak into the chest cavity. This may require a chest tube to re-inflate the lung.
- Nerve Injury: The intercostal nerves run along the bottom of each rib. Damage during surgery can cause chronic neuropathic pain, numbness, or heightened sensitivity (allodynia) along the rib cage and abdomen. This pain can be debilitating and difficult to treat.
- Chest Wall Instability: Removing too much rib or cartilage can theoretically compromise the structural integrity of the chest wall, though this is rare with modern techniques. It can lead to abnormal movement or paradoxical breathing.
- Long-Term Sensory Changes: Permanent numbness or altered sensation in the affected area is common and expected, as nerves are cut. For cosmetic patients, this is a trade-off; for medical patients, it may be an acceptable side effect for pain relief.
- Scarring and Cosmetic Dissatisfaction: The incision scar may be wide, raised (hypertrophic or keloid), or pigmented. The final contour may be asymmetric, or the waist reduction may be less than expected, leading to disappointment.
- Impact on Breathing: While removing a floating rib (11th or 12th) typically has minimal impact on respiratory function, removal of a more anterior rib could potentially affect diaphragmatic attachment and deep breathing mechanics in a small subset of patients.
A thorough risk discussion with your surgeon is non-negotiable. Ask about their specific complication rates and how they manage issues like chronic post-operative pain.
The Cost Factor: A Financial "Before and After"
The financial "before and after" of rib removal is stark. For medically necessary procedures, like a first rib resection for TOS, insurance (including Medicare and Medicaid in the U.S.) often covers a significant portion, as it is considered a treatment for a diagnosed condition. Pre-authorization and documentation of failed conservative therapy are required.
For purely cosmetic rib removal, the patient bears the full cost. This is where the "before and after" has a direct price tag. The total cost can range from $15,000 to $30,000 or more in the United States, depending on:
- Surgeon's Fee: The largest component, based on expertise and reputation. A specialist in chest wall surgery commands a premium.
- Anesthesia Fees.
- Facility Fees: The cost of the operating room and recovery facility.
- Geographic Location: Procedures in major metropolitan areas (New York, Los Angeles) are typically more expensive.
- Extent of Surgery: Removing one rib versus multiple ribs, or combining it with extensive liposuction, increases cost.
- Pre- and Post-Operative Care: Consultations, imaging, follow-up visits, and compression garments.
This high, out-of-pocket cost is a significant barrier and a crucial part of the "before" financial planning. Patients must budget for potential time off work (4-6 weeks for sedentary jobs, longer for physical labor) and any unexpected complication management.
Choosing the Right Surgeon: The Most Critical "Before" Decision
The single most important factor influencing a positive "after" is the surgeon you choose. This is not a procedure for a general plastic surgeon or a discount clinic. You need a specialist with specific, verifiable experience in chest wall surgery.
- Board Certification is the Absolute Minimum: Look for certification by the American Board of Plastic Surgery (ABPS) for cosmetic cases, or the American Board of Thoracic Surgery (ABTS) for medical cases. Verify this status on the official boards' websites.
- Specialized Experience: Ask directly: "How many rib removal procedures (for my specific reason) do you perform annually?" "Can I see before and after photos of your patients with body types similar to mine?" "What is your complication rate for pneumothorax and chronic pain?"
- Hospital Privileges: A qualified surgeon should have operating privileges at an accredited hospital. This is a safety net for managing serious complications.
- Consultation Chemistry: The consultation is your interview. Do they listen? Do they discuss risks as thoroughly as benefits? Do they pressure you, or do they encourage a second opinion? Do they use digital imaging software to simulate potential results? This can help set realistic expectations but is not a guarantee.
- Patient Reviews: Look for patterns in reviews. Multiple complaints about poor bedside manner, unresponsive staff, or unexpected poor outcomes are major red flags.
Choosing the wrong surgeon is the fastest route to a disastrous "after." Invest as much time in this research as you would in buying a house.
Setting Realistic Expectations: The Psychological "Before and After"
Perhaps the most crucial "before" state is your own mindset. Realistic expectations are the bedrock of postoperative satisfaction. Rib removal is a body contouring procedure, not a body transformation.
- It Will Not Make You a Different Person: It will not change your face, your height, or your fundamental proportions. It specifically targets the lower rib cage's width and flare.
- Results Are Subtle to Moderate: Expect a reduction in waist circumference, not a magical 10-inch drop. A 2-4 inch reduction is considered a successful cosmetic outcome. Dramatic, extreme results often involve unhealthy practices or digital manipulation.
- It Complements, It Doesn't Replace, a Healthy Lifestyle: This procedure does not remove fat from your abdomen; it removes bone/cartilage. A healthy diet and core-strengthening exercise are still required to maintain the best possible appearance. Weight gain will still occur in the abdominal area.
- The Scar is Permanent: You will have a scar. Its visibility depends on your genetics, the surgeon's technique, and your scar care regimen (silicone sheets, sun avoidance). It may be hidden by clothing, but it exists.
- Sensation Will Change: Numbness is a guaranteed outcome. For some, this is a minor trade-off; for others, the altered feeling is bothersome.
- Psychological Impact Varies: While many report increased confidence and satisfaction, others experience body dysmorphic disorder (BDD) where the focus simply shifts to another "flaw." A psychological evaluation is sometimes recommended for cosmetic patients to assess for BDD.
The healthiest "after" begins with a "before" where your goals are specific, measurable, and rooted in self-improvement, not self-loathing.
Patient Experiences and Long-Term Outcomes: Voices from the "After"
Beyond statistics and surgeon promises, the lived experiences of patients paint the fullest picture. Long-term outcomes for therapeutic rib removal (e.g., for TOS) are generally positive for pain relief and function, with studies showing 70-80% of patients reporting good to excellent results at 5-year follow-up. However, some may require additional procedures or experience recurrent symptoms.
For cosmetic patients, satisfaction rates are harder to quantify due to a lack of large-scale, long-term studies and the elective nature. Anecdotal reports from online forums and surgeon testimonials suggest a majority are satisfied with their waist reduction, especially when expectations were managed. Common positive themes include: "I can finally wear clothes that fit my waist," "I feel more proportionate," and "the constant self-consciousness about my rib flare is gone."
Conversely, regrets often stem from:
- Unrealistic expectations about the degree of change.
- Inadequate research on the surgeon.
- Underestimation of the pain and recovery duration.
- Permanent numbness or chronic pain that outweighs the aesthetic benefit.
- Scarring that is more prominent than anticipated.
- The psychological realization that changing one body part did not solve deeper self-esteem issues.
The long-term "after" is a mixed landscape. Medically, it can mean pain-free living. Cosmetically, it means a permanently altered skeletal structure with all its sensory and visual consequences. The most successful outcomes are those where the patient entered the process with eyes wide open, a clear medical or aesthetic goal, and a partnership with a supremely qualified surgeon.
Conclusion: Is Rib Removal Right for You?
The journey through "rib removal before and after" reveals a procedure of profound duality. On one hand, it is a powerful therapeutic tool that can liberate patients from the chronic agony of conditions like thoracic outlet syndrome, offering a legitimate "after" of restored function and comfort. On the other, it is an extreme cosmetic intervention that permanently alters the body's fundamental architecture for the sake of an aesthetic ideal, carrying significant risks and a demanding recovery.
The decision to cross the threshold from "before" to "after" cannot be made lightly, based on a single photo or celebrity rumor. It requires:
- A legitimate medical indication or, for cosmetic reasons, a rock-solid, psychologically sound motivation.
- Extensive, critical research to find a surgeon with specific, proven expertise in chest wall surgery.
- A full understanding and acceptance of the risks, including chronic pain, numbness, and a permanent scar.
- Realistic expectations about the degree of change and the permanence of the outcome.
- The financial and temporal resources for the surgery and a full, un-rushed recovery.
If you are considering this procedure, your first step is not to search for more "before and after" pictures, but to schedule consultations with two or three board-certified specialists—a thoracic surgeon for medical concerns, and a highly specialized plastic surgeon for cosmetic ones. Ask every question. Demand to see unedited, timestamped photos of patients with your body type. Most importantly, listen to your own intuition. The right "after" is one built on knowledge, caution, and a decision made from a place of strength, not desperation. Your health and well-being, both physical and mental, are the ultimate outcomes that matter.