How To Crack Your Lower Back Safely: A Complete Guide To Relief And Mobility
Have you ever woken up stiff, twisted after a long drive, or simply felt an uncomfortable ache in your lower spine and thought, “I just need to crack my lower back”? That satisfying pop or release can bring instant, almost magical relief. But how do you do it safely? What does that sound actually mean? And more importantly, is it a long-term solution or just a temporary fix? The desire to crack your lower back is incredibly common, driven by the need for immediate relief from the stiffness and pain that affects a staggering 80% of adults at some point in their lives. This guide dives deep into the mechanics, safe techniques, essential exercises, and critical warnings surrounding lower back manipulation. We’ll move beyond the quick pop to build a foundation for lasting spinal health and mobility, ensuring you understand not just the how, but the why and the when to seek professional help.
Understanding the Science: What Exactly Happens When You "Crack" Your Back?
Before attempting any technique, it’s crucial to understand what that familiar popping sound signifies. It’s not bones grinding or breaking—a common and frightening misconception. The sound, known as crepitus, is primarily caused by a process called cavitation. Within your synovial joints, which include the facet joints of your spine, is a lubricating fluid filled with gases like oxygen, nitrogen, and carbon dioxide. When you stretch a joint quickly, you decrease the pressure within the joint capsule, causing these gases to rapidly form a bubble and "pop." This is similar to opening a bottle of champagne. The bubble then reabsorbs into the fluid over the next 15-30 minutes, which is why you can’t immediately "re-crack" the same spot.
However, the sound can also originate from the stretching of tight ligaments or tendons that snap over bony prominences, or from the friction between cartilage surfaces if there’s any wear. In the lower back, or lumbar spine, the most common joints that produce this sound are the facet joints and sometimes the sacroiliac (SI) joints where the spine meets the pelvis. Understanding this is key because it frames the act not as "adjusting bones back into place"—a dangerous myth—but as releasing gas and mobilizing stiff soft tissues. The feeling of relief comes from the stimulation of nerve endings in the joint capsule, which can temporarily reduce pain signals and increase the range of motion. It’s a neurological reset as much as a mechanical one.
Is It Safe to Crack Your Own Lower Back?
This is the million-dollar question. For the vast majority of people without underlying conditions, self-manipulation of the lumbar spine is generally considered low-risk when done gently and correctly. The real danger lies not in the pop itself, but in the how and the why. Using excessive force, twisting in unnatural ways, or repeatedly forcing a crack on a joint that is already unstable can lead to:
- Ligament sprains from overstretching.
- Muscle strains from guarding or improper form.
- Joint irritation or inflammation.
- In rare cases, if someone has an undiagnosed condition like a herniated disc, spinal stenosis, severe osteoporosis, or a vertebral fracture, aggressive manipulation can exacerbate the problem.
The golden rule: If it hurts to move into the position to crack it, stop. Pain is your body’s primary signal to back off. The goal is a gentle, controlled stretch that may or may not produce a sound, followed by a feeling of release, not a yank that brings sharp pain.
Immediate Relief Techniques: Safe, At-Home Methods for a Quick Release
When you feel that familiar tightness, the goal is to create a gentle stretch and mobilization in the lumbar region. Here are the safest, most effective techniques to try, progressing from simplest to more involved.
- Bellathornedab
- Leaked How To Make A Ribbon Bow So Nude Its Banned Everywhere
- Lotteodditiesxo Exposed Nude Photos And Scandalous Videos Surface Online
1. The Knee-to-Chest Stretch (The Foundational Move)
This is the safest starting point for almost everyone. It gently mobilizes the lumbar spine and pelvis without any twisting forces.
- How to do it: Lie flat on your back on a firm surface, like a mat or carpet. Keep your legs extended and relax. Slowly bend one knee and pull it gently toward your chest, using your hands to clasp just below the kneecap. You should feel a stretch in your lower back and glute. Hold for 20-30 seconds, breathing deeply. Repeat with the other leg. For a deeper stretch, bring both knees to your chest simultaneously, but only if it feels comfortable.
- Why it works: This motion flexes the lumbar spine, creating space between the vertebrae and facet joints, which can allow gas to release. It also stretches the piriformis and gluteus maximus muscles that attach to the sacrum and can contribute to lower back tension.
2. The Seated Spinal Twist
A classic yoga pose that provides a gentle rotational stretch to the entire spine.
- How to do it: Sit on the floor with your legs extended. Bend your right knee and place your right foot flat on the floor outside your left knee. Cross your left elbow over your right knee and gently twist your torso to the right, looking over your right shoulder. Keep your spine long—don’t hunch. You’ll feel a stretch along the left side of your lower back and through the rib cage. Hold for 20-30 seconds, then repeat on the other side.
- Key Tip: The twist should come from your torso, not just your neck. Imagine wringing out a towel from the middle.
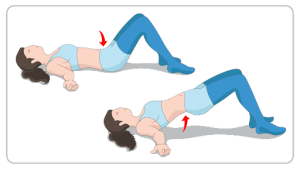
3. The Pelvic Tilt (Engaging Your Core)
This isn’t about cracking, but about activating the deep core muscles (transverse abdominis) that support your lumbar spine. A strong, engaged core can prevent the need to crack in the first place by stabilizing the spine.
- How to do it: Lie on your back with knees bent and feet flat on the floor, hip-width apart. Flatten your lower back against the floor by gently tightening your stomach muscles and tilting your pelvis upward. You should feel your pubic bone move slightly toward your ribs. Hold this engaged position for 5-10 seconds, then release. Perform 10-15 repetitions.
- Why it’s critical: This teaches you to find a neutral spine and builds the muscular corset that protects your discs and joints from everyday stress.
4. Using a Foam Roller for Myofascial Release
Tight thoracolumbar fascia and erector spinae muscles can pull the spine out of alignment, creating the urge to crack. A foam roller can help.
- How to do it: Sit on the floor with a foam roller placed horizontally under your lower back. Support your head with your hands and gently roll up and down, pausing on any particularly tight spots (trigger points) for 20-30 seconds. Crucially, avoid rolling directly over the bony vertebrae of the lumbar spine. Focus on the muscles to the sides (the "kidney" area) and the upper glutes.
- Important Caution: If you have a known disc issue, consult a doctor before using a roller on your lower back.
Building Long-Term Health: Beyond the Quick Pop
Relying solely on self-cracking is like repeatedly hitting the snooze button on an alarm—it provides temporary relief but doesn’t fix the underlying problem. True relief comes from addressing the root causes of stiffness: muscle imbalances, poor posture, weak stabilizers, and lack of movement.
The Core Connection: Why Your Abs and Back Are a Team
Your lumbar spine is inherently unstable. It relies on a deep muscular corset—the transverse abdominis (front), multifidus (along the spine), diaphragm (breathing), and pelvic floor—to create internal pressure and stability. When this "core canister" is weak or inactive, the larger, superficial muscles (like the erector spinae and hip flexors) overcompensate, becoming tight and painful, constantly pulling the spine into unhealthy positions.
- Actionable Strategy: Incorporate core stabilization exercises into your weekly routine. Beyond the pelvic tilt, try:
- Dead Bug: Lying on your back, extend opposite arm and leg while keeping your lower back pressed to the floor.
- Bird-Dog: On all fours, extend opposite arm and leg, maintaining a neutral spine without rotating.
- Plank Variations: Focus on form—a straight line from head to heels, no sagging hips.
The Hip Flexor & Hamstring Duo
Tight hip flexors (psoas, iliacus) pull the pelvis into an anterior tilt, increasing the lumbar curve (hyperlordosis) and compressing the lower vertebrae. Tight hamstrings pull the pelvis into a posterior tilt, flattening the curve and straining the discs. Both create dysfunction.
- Actionable Strategy:
- Hip Flexor Stretch: In a lunge position, tuck your pelvis slightly (posterior tilt) and gently push your hips forward. You should feel a stretch in the front of the hip and thigh of the back leg.
- Hamstring Stretch: Use a dynamic stretch like leg swings (forward and back) or a static stretch lying on your back with a strap around your foot, keeping your knee slightly bent to protect it.
Posture is Everything
Whether you’re at a desk, in a car, or on the couch, sustained slouching puts immense, constant pressure on the lumbar discs and posterior ligaments. The solution isn’t just "sit up straight" (which can be rigid), but to achieve and maintain a neutral spine—where the natural S-curve of the spine is maintained, ears over shoulders, shoulders over hips.
- Ergonomic Fix: Ensure your workstation supports this. Your feet should be flat on the floor, knees at or slightly below hip level, and your monitor at eye level. Use a small lumbar roll or rolled towel to support the natural inward curve of your lower back.
When to Worry: Red Flags and the Importance of Professional Diagnosis
Self-care is powerful, but it has limits. Knowing when to seek a healthcare professional—such as a physiatrist, orthopedic doctor, or a licensed physical therapist—is non-negotiable for your safety. Stop all self-manipulation and consult a doctor immediately if you experience any of the following "red flag" symptoms:
- Severe, unrelenting pain that doesn’t improve with rest.
- Pain, numbness, or weakness radiating down one or both legs (sciatica symptoms).
- Loss of bowel or bladder control (a sign of cauda equina syndrome—a medical emergency).
- Unexplained weight loss or fever accompanying back pain.
- History of cancer or recent infection.
- Pain that is worse at night and disrupts sleep.
- A traumatic injury (like a fall or car accident) preceding the pain.
These symptoms can indicate serious conditions like cauda equina syndrome, spinal infection, tumor, or an unstable fracture that require immediate medical intervention.
The Role of the Physical Therapist and Chiropractor
A physical therapist (PT) is your best first stop for most non-emergency back issues. They are movement experts who will:
- Perform a detailed assessment to identify muscle imbalances and movement dysfunctions.
- Provide manual therapy (safe, targeted joint and soft tissue mobilization).
- Design a personalized exercise program to correct your specific weaknesses.
- Educate you on posture and body mechanics.
A chiropractor specializes in spinal manipulation therapy (SMT). If you choose this route, ensure they are licensed and reputable. A good chiropractor will:
- Take a thorough history and perform/order necessary imaging (X-rays, MRI) before adjusting.
- Use a variety of techniques, not just high-velocity thrusts.
- Provide exercises and advice for home care.
- Refer you out if they suspect a condition outside their scope.
Debunking Common Myths About Cracking Your Back
Let’s separate fact from fiction, as myths can lead to harmful habits.
- Myth: Cracking your back causes arthritis.
- Fact: There is no scientific evidence linking joint cracking to osteoarthritis. The cavitation process does not wear down cartilage. However, repeatedly forcing a joint that is already unstable or painful can accelerate wear over time—so it’s about how you do it, not the sound itself.
- Myth: You need to crack your back to put a "subluxated" vertebra back in place.
- Fact: The concept of a vertebra being "out of place" and needing to be "put back" is largely a chiropractic myth not supported by radiological evidence. The spine is a stable, robust structure. The feeling of relief comes from muscle relaxation and nerve desensitization, not from moving a bone.
- Myth: If it doesn’t crack, the stretch isn’t working.
- Fact: The pop is incidental. A stretch can be profoundly beneficial and therapeutic without any sound. Focus on the feeling of lengthening and release in the muscles, not on achieving a pop.
- Myth: Cracking your own back is just as good as seeing a professional.
- Fact: Professionals have years of training to identify specific joint restrictions, assess your whole-body mechanics, and apply a precise, controlled force where it’s needed. You are guessing; they are diagnosing. Self-cracking often targets the wrong, hypermobile segments above or below the true stiff joint, potentially creating more instability.
Your Action Plan: A 4-Week Path to a Healthier Lower Back
Instead of a daily habit of seeking cracks, follow this structured plan for sustainable relief.
Week 1-2: Awareness & Foundation
- Stop all aggressive, forceful cracking.
- Practice the Knee-to-Chest and Pelvic Tilt exercises 2-3 times daily.
- Begin a daily 5-minute mindful posture check. Set phone reminders.
- Start a gentle walking routine (20-30 minutes daily). Walking pumps fluids through the spinal discs, nourishing them.
Week 3-4: Integration & Strengthening
- Add the Seated Spinal Twist and Hip Flexor/Hamstring stretches to your routine.
- Introduce core stabilization: Start with 2 sets of 10 Dead Bugs and Bird-Dogs every other day.
- If pain persists, schedule an appointment with a physical therapist for a professional assessment.
- Invest in a lumbar support pillow for your office chair and car.
Beyond 4 Weeks: Maintenance
- Make core work and stretching a non-negotiable part of your weekly routine (3-4 times a week).
- Continue posture vigilance.
- Consider activities like swimming, Pilates, or yoga that build core strength and spinal mobility holistically.
Conclusion: Empowerment Over Impulse
The urge to crack your lower back is a signal from your body—a signal of stiffness, imbalance, and a need for movement. By understanding the science behind the pop, you demystify the process and remove the anxiety. By learning the safe, gentle techniques like the knee-to-chest and pelvic tilt, you have tools for immediate, responsible relief. But the true power lies in shifting your focus from a fleeting pop to long-term resilience. This means building a strong, supportive core, stretching tight hip and back muscles, and mastering neutral posture in daily life.
Your lower back is a powerhouse of movement and stability. Treat it not as a joint to be forcibly adjusted, but as a complex system to be nurtured with strength, flexibility, and intelligent movement. If the pain is persistent, severe, or accompanied by red flags, consult a healthcare professional without hesitation. A physical therapist can be your greatest ally, providing a personalized roadmap to a back that feels strong, mobile, and free—a back you don’t feel the need to crack because it’s already working perfectly for you. Start with awareness, move with intention, and build a foundation of health that lasts a lifetime.