Can Your Diet Really Trigger Appendicitis? The Surprising Truth About Food And Appendix Health
Have you ever wondered, "what food can cause appendicitis?" It’s a question that likely crosses your mind when you hear about someone rushing to the hospital with severe abdominal pain. Appendicitis—the inflammation of the appendix—is a common surgical emergency, but its exact cause often remains a mystery. While we know blockages from hardened stool (fecaliths) are a primary culprit, could the foods we eat be setting the stage for that blockage? The relationship between diet and appendicitis isn't about a single "bad" food causing instant trouble. Instead, it's about long-term dietary patterns that may increase the risk of obstruction and inflammation. Let's cut through the myths and explore the science-backed connections between what's on your plate and the health of your appendix.
Understanding the Appendix: More Than Just a Useless Vestige
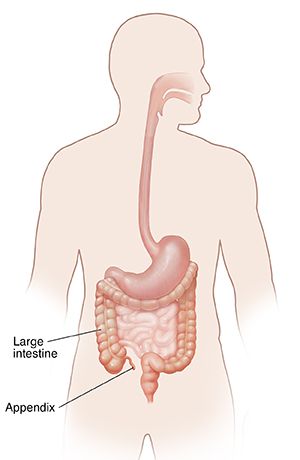
Before diving into food, it's crucial to understand what the appendix actually is. For years, it was dismissed as a vestigial organ with no real purpose. Modern research, however, suggests it may play a role in gut immunity and as a "safe house" for beneficial gut bacteria. It's a narrow, finger-sized pouch branching off the large intestine. Its structure—a small opening leading into a blind-ended tube—makes it uniquely vulnerable. Anything that obstructs this narrow lumen can trap bacteria and fluids, leading to swelling, reduced blood flow, and ultimately, inflammation and rupture if untreated.
The classic cause is a fecalith—a hard piece of stool—that lodges at the entrance. But what contributes to the formation of these obstructions? This is where diet enters the picture. A diet consistently low in fiber and high in processed foods can slow down digestion and lead to harder, drier stools. Over time, this environment increases the likelihood of a piece getting stuck. It’s not a direct, immediate cause-and-effect like food poisoning, but a gradual process of creating the right conditions for a problem to arise.
The Low-Fiber Diet: A Major Contributor to Appendix Obstruction
How Fiber Keeps Things Moving
Dietary fiber is the indigestible part of plant foods that adds bulk to stool and promotes regular bowel movements. There are two types: soluble fiber (dissolves in water, forms a gel) and insoluble fiber (adds bulk, speeds up passage). Both are critical for colon health. A diet rich in fruits, vegetables, whole grains, legumes, nuts, and seeds ensures that waste moves smoothly through the digestive tract, preventing stagnation and hardening.
The Western Diet Pattern and Its Risks
Numerous epidemiological studies have linked a Western dietary pattern—characterized by high intake of refined grains, red and processed meats, high-fat dairy products, and sugary foods, and low intake of fruits, vegetables, and whole grains—to an increased risk of appendicitis. One significant study published in the European Journal of Clinical Nutrition found that low fiber intake, particularly from fruits and vegetables, was associated with a higher incidence of appendicitis. The mechanism is straightforward: without sufficient fiber, transit time through the colon slows, allowing more water to be absorbed from the stool. This results in smaller, harder pellets that are more likely to form a plug at the appendix's opening.
Practical Tip: Aim for 25-30 grams of fiber daily. Start your day with oatmeal topped with berries and a tablespoon of flaxseeds. Choose whole-wheat bread over white, and incorporate legumes like lentils or beans into salads and soups a few times a week. Increase fiber intake gradually and drink plenty of water to help it work effectively.
- Tennis Community Reels From Eugenie Bouchards Pornographic Video Scandal
- Breaking Cdl Intel Twitter Hacked Sex Tapes Leaked Online
- Kaliknockers
Seeds, Nuts, and Popcorn: Are They Really the Enemy?
The Persistent Myth
For decades, a common piece of advice given to children was to avoid swallowing seeds (like from strawberries, kiwi, or tomatoes), nuts, and popcorn because they could get stuck in the appendix. This myth caused unnecessary anxiety and dietary restrictions. The logic seems sound—small, hard particles could theoretically lodge in the narrow opening.
What the Science Says
The scientific consensus, backed by major health organizations like the American Academy of Pediatrics and the National Institutes of Health, is that there is no evidence to support this claim. A study published in JAMA Pediatrics specifically examined children who had appendectomies and found no correlation between the consumption of seeds, nuts, or popcorn and the development of appendicitis. The appendix's opening is generally wide enough to allow these small, indigestible bits to pass through without issue. The real risk comes from larger, aggregated pieces of hardened stool, not individual seeds or popcorn kernels.
Key Takeaway: Don't fear the seeds in your raspberries or the nuts in your granola. The benefits of these nutrient-dense foods far outweigh this unsubstantiated risk. Focus your concern on overall fiber intake instead.
Processed Foods and Red Meat: The Inflammatory Connection
The Role of Pro-Inflammatory Diets
A diet high in processed foods (chips, fast food, frozen meals, packaged snacks) and red/processed meats (bacon, sausage, deli meats) is often low in fiber and high in unhealthy fats, sodium, and preservatives. Such a diet can promote systemic inflammation throughout the body, including in the gastrointestinal tract. Chronic, low-grade inflammation may alter the gut microbiome and environment, potentially making the appendix more susceptible to infection and obstruction once a blockage occurs.
Furthermore, high meat consumption, especially when cooked at high temperatures (grilling, frying), can produce compounds like heterocyclic amines (HCAs) and polycyclic aromatic hydrocarbons (PAHs), which may have inflammatory effects. While not a direct cause, this pattern contributes to an overall gut health profile that is less resilient.
The Fat Factor
High intake of saturated and trans fats is associated with slower gut motility and can contribute to the formation of denser, more difficult-to-pass stool. A sluggish colon is a colon where things can get stuck.
Actionable Advice: Limit processed meats to occasional treats. When eating red meat, choose lean cuts and use gentler cooking methods like baking or stewing. Swap processed snacks for whole-food alternatives like an apple with almond butter or carrot sticks with hummus.
Foodborne Illness and Gut Health: An Indirect Link
Pathogens and Obstruction
While not a direct "cause," severe cases of food poisoning or gastroenteritis caused by pathogens like Salmonella, Campylobacter, or certain parasites can lead to intense inflammation and swelling of the lymphoid tissue in the appendix and surrounding areas. In rare cases, this swelling itself can cause a functional obstruction, even without a fecalith. This is more of an acute trigger in a predisposed individual rather than a chronic dietary cause.
The Microbiome Factor
Your long-term diet shapes your gut microbiome—the trillions of bacteria living in your intestines. A diverse, fiber-fed microbiome is associated with better gut health and regular motility. A diet low in fiber and high in sugar and processed foods can reduce microbial diversity and promote the growth of potentially harmful bacteria. An imbalanced microbiome may influence the consistency of stool and the health of the intestinal lining, indirectly affecting appendix risk.
Proactive Step: Incorporate fermented foods like yogurt (with live cultures), kefir, sauerkraut, and kimchi into your diet to support a healthy gut flora. These foods introduce beneficial bacteria that can aid digestion and overall gut ecosystem balance.
Dehydration: The Overlooked Culprit
How Water Prevents Hard Stools
Adequate hydration is non-negotiable for preventing constipation and maintaining soft, bulky stool. Fiber works by absorbing water. If you're dehydrated, even a high-fiber diet can backfire, leading to hard, dry stools that are difficult to pass. Chronic dehydration is a significant, often overlooked, risk factor for fecalith formation.
Signs You're Not Drinking Enough
Beyond thirst, signs of dehydration include dark yellow urine, infrequent urination, fatigue, dizziness, and, most relevantly, hard or lumpy stools (types 1-2 on the Bristol Stool Chart). Many people simply don't drink enough water throughout the day.
Simple Habit: Carry a reusable water bottle and aim to drink at least 2 liters (8 cups) of water daily, more if you are active or live in a hot climate. Herbal teas and water-rich foods like cucumber and watermelon also contribute to your fluid intake.
Putting It All Together: An Appendix-Friendly Diet
So, what does a diet that supports appendix and overall colon health look like? It’s not about restrictive elimination but about embracing a pattern of abundance:
- Load Up on Fiber: Make plants the star of every meal. Aim for a rainbow of colors to get a wide array of nutrients and fiber types.
- Choose Healthy Fats: Opt for fats from avocados, olive oil, nuts, and seeds instead of saturated fats from fatty meats and fried foods.
- Prioritize Whole Foods: Eat foods as close to their natural state as possible. An apple is better than apple juice; a baked potato is better than potato chips.
- Stay Hydrated: Water is your best friend for digestive health.
- Limit Processed Intake: Significantly reduce consumption of packaged snacks, sugary drinks, fast food, and processed meats.
- Include Probiotics: Support your gut bacteria with fermented foods or a supplement if needed.
This pattern is essentially the Mediterranean diet, which is consistently linked to lower risks of numerous chronic diseases, including colorectal issues.
Beyond Diet: Other Risk Factors for Appendicitis
It’s important to remember that diet is just one piece of the puzzle. Appendicitis can occur in anyone with an appendix, regardless of diet. Other significant risk factors include:
- Age: Most common between 10-30 years old.
- Family History: Having a first-degree relative with appendicitis increases your risk.
- Obstruction from Other Sources: Sometimes, the blockage is from a foreign body, a tumor (more common in older adults), or swollen lymph nodes from an infection elsewhere in the body.
- Trauma: Rarely, abdominal injury can contribute.
This is why it’s critical to know the symptoms: sudden pain that begins around the navel and shifts to the lower right abdomen, loss of appetite, nausea, vomiting, low-grade fever, and abdominal swelling or rigidity. If you experience these, seek medical attention immediately. Do not wait, and do not rely on dietary changes to treat an active case.
Conclusion: Empower Your Choices, Not Your Fear
The question "what food can cause appendicitis?" leads us to a nuanced answer. No single food is a guaranteed trigger. Instead, the long-term pattern of a low-fiber, high-processed-food diet creates a digestive environment—sluggish motility, harder stools, potential inflammation—that may increase the statistical likelihood of the appendix becoming obstructed. Conversely, a diet rich in fiber, hydration, and whole plants promotes regular bowel movements and a healthier gut ecosystem, which is your best dietary defense.
Ultimately, focusing on an appendix-friendly diet is simply focusing on an overall healthy diet. The principles—more plants, plenty of water, fewer processed items—are the same ones that protect your heart, help maintain a healthy weight, and reduce the risk of type 2 diabetes and certain cancers. You don’t need to live in fear of seeds or nuts. Instead, empower yourself with consistent, positive dietary habits that support your entire digestive system, appendix included. If you have concerns about your personal risk, especially with a family history, discuss them with your doctor. But for most people, the path to a healthier appendix is the same path to a healthier you: a plate full of color, a glass full of water, and a commitment to whole, nourishing foods.