How Many Ultrasounds During Pregnancy? A Complete Guide To Prenatal Scans
How many ultrasounds during pregnancy will you actually have? This simple question often sparks a mix of excitement and anxiety for expectant parents. The ultrasound is one of the most magical moments of pregnancy—the first time you see your baby, hear their heartbeat, and witness their tiny movements. But beyond the emotional milestone, ultrasounds are critical medical tools. The number isn't arbitrary; it's a carefully considered part of your prenatal care plan designed to monitor your health and your baby's development. This comprehensive guide will walk you through everything you need to know about the typical ultrasound schedule, the different types of scans, why your doctor might recommend more or fewer, and the essential safety facts, giving you a clear picture of what to expect on this journey.
Understanding the Role of Prenatal Ultrasounds
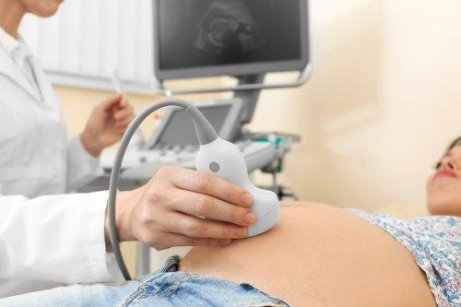
Before diving into the numbers, it's helpful to understand what an ultrasound is and why it's used. An ultrasound, or sonogram, is a diagnostic imaging technique that uses high-frequency sound waves to create real-time images of your developing baby, the placenta, and your uterus. A handheld device called a transducer sends sound waves into your abdomen (or vagina for early scans); these waves bounce back and are translated into a picture on a screen. This non-invasive, radiation-free technology is the primary method for assessing fetal growth, anatomy, position, and overall well-being throughout pregnancy.
Healthcare providers rely on ultrasounds for several key reasons. They confirm the pregnancy, establish gestational age, and detect multiple fetuses. They screen for potential birth defects or anatomical abnormalities, monitor the baby's growth rate, check the placenta's location and health, and assess amniotic fluid levels. For parents, it's an irreplaceable bonding experience. The American College of Obstetricians and Gynecologists (ACOG) endorses the use of ultrasounds when medically indicated, emphasizing that they should be performed for valid clinical reasons rather than as a routine, non-essential part of every prenatal visit. The principle of "ALARA" (As Low As Reasonably Achievable) guides their use, ensuring the lowest possible exposure time and intensity needed to get a diagnostic image.
- Chloe Parker Leaks
- Exclusive Leak The Yorkipoos Dark Secret That Breeders Dont Want You To Know
- Explosive Thunder Vs Pacers Footage Leaked Inside The Shocking Moments They Tried To Hide
The Standard Ultrasound Schedule: A Trimester-by-Trimester Breakdown
So, how many ultrasounds during pregnancy are considered standard in a low-risk, uncomplicated pregnancy? While individual practices and insurance plans vary, a common schedule endorsed by many obstetricians includes two to three key ultrasounds. Here is the typical timeline, broken down by trimester.
First Trimester Ultrasound (Weeks 6-13)
The first ultrasound is often the most anticipated. It's typically performed between 6 to 9 weeks and is sometimes called a "dating scan." Its primary purposes are to:
- Confirm an intrauterine pregnancy (ruling out ectopic pregnancy).
- Detect a fetal heartbeat.
- Measure the gestational sac and crown-rump length (CRL) to establish an accurate due date. This is crucial, as it becomes the benchmark for all future growth assessments.
- Identify if you are carrying multiples (twins, triplets, etc.).
- For those who conceived via IVF, this scan confirms the number of gestational sacs.
For many, this early scan is transvaginal (using a slender probe inserted into the vagina) because the uterus is still small and deep in the pelvis, providing a clearer image. This scan is not always routine for every low-risk pregnancy; some providers may wait until the 11-14 week window for the nuchal translucency scan unless there are symptoms like bleeding or pain.
- Twitter Erupts Over Charlie Kirks Secret Video Leak You Wont Believe Whats Inside
- The Turken Scandal Leaked Evidence Of A Dark Secret Thats Gone Viral
- Will Ghislaine Maxwell Make A Plea Deal
Second Trimester Ultrasound (The Anatomy Scan, Weeks 18-22)
This is the most comprehensive and detailed ultrasound of pregnancy, often referred to as the "anatomy scan" or "level 2 ultrasound." It is almost universally recommended between 18 and 22 weeks, with 20 weeks being the sweet spot. At this stage, the baby's organs and structures are developed enough to be thoroughly examined. A sonographer will systematically check:
- Brain and Spine: Looking for neural tube defects like spina bifida.
- Heart: Assessing the four chambers, rhythm, and major blood vessels.
- Face: Checking for cleft lip/palate.
- Abdomen: Examining the stomach, bladder, kidneys, and diaphragm.
- Limbs: Confirming arms, legs, hands, and feet are present and formed.
- Placenta and Cervix: Checking location (to rule out placenta previa) and cervical length.
- Amniotic Fluid Volume: Ensuring it's within a normal range.
This scan can take 30-45 minutes or longer. If any potential soft markers or minor abnormalities are seen, a follow-up scan or a referral to a maternal-fetal medicine (MFM) specialist may be recommended. This is also often when parents can find out the baby's sex, if they choose.
Third Trimester Ultrasound (Growth Scan, Weeks 28-40)
A third-trimester ultrasound, or "growth scan," is not always routine for every low-risk pregnancy. ACOG states it may be performed between 28 and 32 weeks to assess fetal growth, amniotic fluid, and placental position, especially if there are concerns like maternal hypertension, diabetes, or if the fundal height measurement (the tape measure around your belly) is not matching the gestational age. Its goals are to:
- Measure the baby's head, abdomen, and femur bone to estimate weight.
- Check the baby's position (head-down, breech, transverse).
- Reassess the placenta's location and appearance.
- Evaluate amniotic fluid levels.
- Observe fetal movement and breathing motions.
For some providers, a final scan around 36-37 weeks may be done to get a final growth estimate and position before labor.
Typical Ultrasound Schedule Summary:
| Trimester | Timing (Weeks) | Primary Purpose | Common Name |
|---|---|---|---|
| First | 6-9 (or 11-14) | Dating, heartbeat, confirmation | Dating Scan / NT Scan |
| Second | 18-22 | Detailed anatomy survey | Anatomy Scan / Level 2 |
| Third | 28-32 (optional) | Growth, fluid, position | Growth Scan |
Beyond the Basics: Specialized and Optional Ultrasounds
The standard schedule is a guideline. Many pregnancies require additional, specialized ultrasounds for various medical reasons. Furthermore, some parents choose optional, non-medical scans for bonding purposes. It's important to distinguish between the two.
Medically Necessary Additional Scans
If you have a high-risk pregnancy (due to pre-existing conditions like hypertension or diabetes, pregnancy complications like preeclampsia or gestational diabetes, or issues identified in earlier scans), your provider will likely order more frequent ultrasounds. For example:
- Weekly or Biweekly Growth Scans: For suspected growth restriction (IUGR) or macrosomia (large baby).
- Doppler Ultrasound: This specialized ultrasound measures blood flow in the umbilical artery, middle cerebral artery, and uterine arteries. It's used to assess how well the baby is being oxygenated and nourished, often in cases of IUGR, maternal hypertension, or diabetes.
- Biophysical Profile (BPP): This is a combination test that includes a non-stress test (NST) and an ultrasound to assess fetal breathing, movement, muscle tone, and amniotic fluid. It's commonly used in the third trimester for ongoing fetal surveillance.
- Follow-up Scans: To monitor a known issue, like a placenta previa that may resolve, a congenital anomaly, or a twin-to-twin transfusion syndrome in monochorionic twins.
Optional "Keepsake" or "3D/4D" Ultrasounds
These are elective scans offered by private studios, usually between 26-34 weeks, that provide 3D (still images) and 4D (video) views of the baby's face. Major medical organizations, including ACOG and the FDA, caution against these for non-medical reasons. The primary concerns are:
- Lack of Medical Oversight: These facilities may not have a licensed physician interpreting the images, potentially missing subtle abnormalities.
- Excessive Exposure: While diagnostic ultrasounds are considered safe, the "dose" of sound waves is kept as low as possible. Prolonged sessions for entertainment purposes contradict the ALARA principle.
- False Reassurance or Alarm: A beautiful 3D image does not guarantee a healthy baby, as internal organs are not being thoroughly assessed.
If you choose to have one, ensure it's performed by a qualified sonographer under the guidance of your physician, and never use it as a substitute for your medically indicated anatomy scan.
Factors That Influence Your Personal Ultrasound Count
The answer to "how many ultrasounds during pregnancy" is ultimately personalized. Your specific number depends on a matrix of factors that your healthcare provider continuously assesses. Here are the primary determinants:
- Pregnancy Risk Status: This is the biggest factor. A low-risk, singleton pregnancy with no prior complications may stick to the 2-3 scan schedule. A high-risk pregnancy can easily involve 6, 8, or more scans.
- Maternal Health Conditions: Pre-existing or gestational diabetes, chronic hypertension, kidney disease, or autoimmune disorders often necessitate closer monitoring via ultrasound.
- Previous Pregnancy History: A history of preterm birth, stillbirth, or a child with a genetic condition may lead to more surveillance.
- Fetal Findings: Any soft marker, growth concern, or suspected anomaly from the anatomy scan will trigger a follow-up scan, often with a specialist.
- Multiple Gestation: Twins, triplets, or more automatically increase the frequency. Monochorionic (sharing a placenta) twins require very close monitoring with Doppler scans to check for twin-to-twin transfusion syndrome.
- Patient Anxiety and Request: While not a primary medical reason, some providers may order an extra scan if a patient is experiencing significant anxiety about fetal movement or well-being, especially after a loss. It's always okay to discuss your concerns with your doctor.
- Provider and Facility Protocols: Practices and hospitals have their own standard protocols based on their patient population and resources.
The Safety of Ultrasounds: Separating Myth from Fact
A common and understandable worry is: "Are all these ultrasounds safe for my baby?" The overwhelming consensus from decades of research and major health bodies is that diagnostic ultrasounds are safe when used appropriately. Unlike X-rays or CT scans, ultrasounds use sound waves, not ionizing radiation. There is no evidence that the use of ultrasound during pregnancy causes harm to the fetus or the mother.
However, this safety is predicated on the "as low as reasonably achievable" (ALARA) principle. The ultrasound machine's power output is limited by law (the FDA regulates the acoustic output), and sonographers are trained to minimize scan time while obtaining the necessary diagnostic information. The biological effects of ultrasound are primarily thermal (heating) and mechanical (pressure). At the low intensities used for diagnostic imaging, these effects are negligible and have not been shown to cause harm in human studies.
The key takeaway is that the benefit of a medically necessary ultrasound always outweighs any theoretical risk. The risk of not diagnosing a serious condition like a placenta previa or severe growth restriction far exceeds the minuscule, unproven risk from the scan itself. The caution against non-medical "keepsake" scans is purely a precautionary measure to avoid unnecessary exposure, not because they are known to be dangerous.
Addressing Your Top Questions About Pregnancy Ultrasounds
Let's tackle the most common questions that arise when parents ponder their ultrasound journey.
Q: Can I refuse an ultrasound?
A: Yes, you have the right to refuse any medical procedure, including ultrasounds. However, it's crucial to have a thorough discussion with your provider about the specific medical reason for the recommended scan. For instance, refusing the anatomy scan means you forgo the most comprehensive screen for major birth defects. Refusing a growth scan for a suspected growth-restricted baby could mean missing a sign that the baby needs early delivery. Informed refusal means understanding the potential consequences of not having the information the scan provides.
Q: What if an abnormality is found?
A: If a potential issue is detected on an ultrasound, it is not a diagnosis. It's a "soft marker" or finding that warrants further investigation. Your provider will likely refer you to a maternal-fetal medicine (MFM) specialist. The next steps may include a more detailed, high-resolution ultrasound, genetic counseling, and possibly invasive tests like amniocentesis or chorionic villus sampling (CVS) to get a definitive chromosomal or genetic diagnosis. Many "abnormalities" seen on screening ultrasounds turn out to be normal variations or resolve on their own.
Q: How should I prepare for my ultrasound?
A: Preparation depends on the type and timing.
- First Trimester (Transvaginal): You typically need a full bladder to lift the uterus for a better abdominal view, but for a transvaginal scan, an empty bladder is best. Your clinic will give specific instructions.
- Second/Third Trimester (Abdominal): You will almost always need a full bladder. Drink 32 ounces of water 1 hour before your appointment and do not urinate. A full bladder acts as a "window" for the sound waves and pushes the intestines out of the way. Wear comfortable, loose-fitting clothing that can be easily pulled up.
- General: Bring your questions! Have a list ready for the sonographer or doctor. While sonographers can't diagnose or give medical advice, they can often point out anatomy if they are allowed to by your provider's policy.
Q: Do I need a full bladder for every scan?
A: Almost always for abdominal scans in the 2nd and 3rd trimesters. For very early transvaginal scans, you may be asked to empty your bladder. Always follow the specific instructions given by your imaging center, as protocols vary.
Q: What's the difference between 2D, 3D, and 4D?
A: 2D is the standard, flat, black-and-white image used for all diagnostic measurements. 3D adds a third dimension, creating a still, shaded image that looks more like a photograph. 4D is 3D in motion, adding the element of time. 3D/4D can be helpful in visualizing certain facial or limb abnormalities that are harder to see in 2D, but 2D remains the gold standard for a complete, systematic anatomical survey because it allows the sonographer to see through the baby to examine internal organs.
Conclusion: Partnering with Your Healthcare Team
So, how many ultrasounds during pregnancy will you have? The answer lies in a collaborative conversation with your obstetrician or midwife. The standard blueprint of a dating scan, an anatomy scan, and possibly a growth scan provides a solid foundation for most low-risk pregnancies. However, your personal journey is unique. Factors like your health history, the baby's development, and any arising complications will shape your individual schedule.
Remember, each ultrasound serves a purpose—whether it's to date the pregnancy, reassure you with a strong heartbeat, perform a life-saving anatomical check, or monitor a known condition. They are powerful tools that provide invaluable peace of mind and critical medical information. Trust the process, ask questions, and understand the "why" behind each recommended scan. By staying informed and working as a partner with your prenatal care team, you can navigate your ultrasound schedule with confidence, focusing on the joy of each glimpse of your growing baby while ensuring the highest standard of medical care for both of you. The number on its own is less important than the quality of information and care each scan provides.