Panniculectomy Before And After: Your Complete Guide To Transformation
Have you ever looked in the mirror and wondered, "What would my life be like if that heavy, uncomfortable apron of skin and tissue was gone?" The journey of a panniculectomy before and after is one of the most profound physical and emotional transformations in cosmetic and reconstructive surgery. It’s more than just a procedure; it’s the removal of a literal weight that has held you back, impacting everything from your ability to exercise comfortably to your self-confidence in a fitted shirt. This comprehensive guide will walk you through every single stage, from the initial consultation to the stunning final results, giving you a clear, honest picture of what to expect. We’ll delve into the medical realities, the recovery timeline, and showcase real panniculectomy before and after photos to illustrate the remarkable change. If you’re considering this life-changing excess skin removal surgery, understanding the full spectrum—from the pre-operative checklist to the long-term outcome—is the first and most crucial step.
Understanding the Panniculectomy: More Than Just a Tummy Tuck
Before we dive into the "before and after," it’s essential to understand exactly what a panniculectomy is and how it differs from its more famous cousin, the abdominoplasty (tummy tuck). While both procedures address the abdominal area, their primary goals and techniques are distinct.
A panniculectomy is a surgical procedure specifically designed to remove the pannus—the medical term for the large, overhanging fold of skin and fat that hangs from the lower abdomen. This is often a consequence of significant weight loss, whether from bariatric surgery, diet, or exercise, or it can be present after multiple pregnancies. The pannus can cause chronic skin irritation, rashes, infections (like cellulitis), difficulty with hygiene, and severe mobility issues. The primary goal of a panniculectomy is functional relief and hygiene improvement. It removes this heavy, troublesome apron.
- Why Is The Maxwell Trial A Secret Nude Photos And Porn Leaks Expose The Cover Up
- Reagan Gomez Prestons Shocking Leak The Video That Destroyed Her Career
- Knoxville Marketplace
In contrast, a tummy tuck is more of a cosmetic contouring procedure. It removes a smaller amount of excess skin and fat but, crucially, also tightens the underlying abdominal muscles (rectus diastasis) that may have separated and weakened. A tummy tuck reshapes and flattens the entire abdomen for aesthetic enhancement. Many patients who have lost a massive amount of weight may need a combination procedure—often called an "extended abdominoplasty" or "body lift"—which addresses both the functional pannus and the muscular laxity for a complete transformation.
Who is the Ideal Candidate?
The ideal candidate for a standalone panniculectomy is someone who:
- Has a significant overhanging pannus that causes physical discomfort, skin breakdown, or recurrent infections.
- Has achieved and maintained a stable weight for at least 6-12 months post-weight loss.
- Is in good general health, with no uncontrolled conditions like diabetes or heart disease that could impair healing.
- Is a non-smoker or is willing to quit smoking well before surgery, as nicotine severely compromises blood flow and wound healing.
- Has realistic expectations about scarring and the recovery process.
A thorough consultation with a board-certified plastic surgeon is non-negotiable. They will assess your specific anatomy, the quality of your skin, the extent of the pannus, and your overall health to determine if a panniculectomy alone is sufficient or if a more extensive body contouring procedure is recommended.
- Popes Nude Scandal Trumps Explosive Allegations Exposed In New Leak
- Will Poulter Movies Archive Leaked Unseen Pornographic Footage Revealed
- Stuart Mad Tv Leak Secret Video Reveals His Darkest Secret
The "Before": Preparation and Anticipation
The period leading up to your surgery date is critical for setting the stage for a successful outcome. This "before" phase is about optimization, planning, and mental preparation.
The Initial Consultation: Laying the Groundwork
Your first meeting with the surgeon is a two-way conversation. Be prepared to discuss:
- Your complete medical history, including all medications, supplements, and allergies.
- Your history of weight fluctuations and any previous abdominal surgeries.
- Your specific symptoms: Do you get rashes? Is it difficult to walk or exercise? How does it affect your daily life?
- Your aesthetic goals. Even though the primary aim is functional, most patients also hope for a flatter, smoother abdominal contour.
The surgeon will perform a physical exam, assess your skin’s elasticity, and may take standardized panniculectomy before photos from multiple angles. These photos are crucial for surgical planning and for you to later appreciate the panniculectomy after results. They will explain the surgical technique, the location and expected length of the incision (typically a horizontal line low on the abdomen, from hip to hip), the need for possible liposuction to contour the flanks, and whether a secondary procedure to tighten muscles might be needed.
Pre-Operative Checklist: Getting Your Body Ready
In the weeks and months leading to surgery, you will be given a detailed pre-op plan. This often includes:
- Medical Optimization: Your surgeon may require lab work, an EKG, or clearance from your primary care physician or a specialist if you have chronic conditions.
- Medication Management: You will be advised to stop taking certain medications that increase bleeding risk, such as aspirin, ibuprofen, and some herbal supplements (e.g., ginkgo, garlic pills, high-dose vitamin E). Your doctor will provide a precise list.
- Lifestyle Adjustments: This is the time to commit to a healthy, protein-rich diet to support healing. If you smoke, you must quit at least 4-6 weeks before and after surgery. Hydration is key.
- Practical Arrangements: You will need to arrange for someone to drive you home and stay with you for at least the first 24-48 hours. Prepare your recovery space in advance—a comfortable recliner, easy-to-wear clothing (button-down shirts, loose pants), pre-made meals, and items within easy reach to minimize bending and stretching.
- Mental Preparation: Understand that you will be swollen and bruised immediately after. The final result takes many months to emerge as swelling subsides and scars mature. Patience is part of the process.
The Surgical Journey: What Happens on the Day
On the day of your panniculectomy surgery, you’ll arrive at an accredited surgical facility or hospital. The procedure is typically performed under general anesthesia and can take 2 to 4 hours, depending on the complexity.
The surgeon makes a low, horizontal incision, carefully designed to be concealed by most clothing and swimwear. They then meticulously elevate the skin and fat of the pannus away from the underlying abdominal wall fascia. The excess tissue is carefully trimmed away, and the remaining skin is pulled downward and sutured closed, creating a smoother, flatter abdominal profile. If liposuction is part of the plan to address the love handles or flanks, it is often performed at this stage. Drains are usually placed to prevent fluid accumulation (seroma) under the incision. The incision is closed in layers with dissolvable sutures beneath the skin and removable sutures or staples on the surface.
You will wake up in the recovery room with a bulky dressing and possibly a compression garment already in place. You will feel tightness, soreness, and significant swelling. Pain will be managed with prescribed medications. The initial panniculectomy before and after contrast is immediate and dramatic, but it is only the very beginning of the healing story.
The "After": Recovery and the Road to Final Results
The recovery phase is where your dedication to the pre-op instructions pays off. It’s a process of patience and careful healing, typically broken down into phases.
The First Few Weeks: Rest and Initial Healing
The first 1-2 weeks are about rest and managing the initial discomfort. You will have drains in place, which you or a caregiver will need to monitor and record the output. Your movement will be severely limited; you will be taught how to get in and out of bed using a "log roll" technique to avoid straining your incision. Walking short distances around your home is encouraged to promote circulation and prevent blood clots, but absolutely no lifting, bending, or twisting.
- Week 1: You’ll have your first post-op visit. Sutures or staples may be removed, and drains will likely come out when output is minimal (usually within 1-3 weeks). Swelling and bruising will be at their peak.
- Weeks 2-4: You’ll gradually increase activity, moving from short, supported walks to slightly longer ones. You may return to a sedentary desk job around 2-3 weeks, but listen to your body. The compression garment must be worn almost constantly (23 hours a day) for the first several weeks to control swelling and support the tissues as they heal.
- Weeks 4-6: Many patients feel comfortable resuming light household duties. You may be cleared for light, low-impact exercise like short walks, but no core workouts, running, or weightlifting. The incision will still be tender and numb.
Months 2-6: Swelling Subsides, Scars Mature
This is a period of visible improvement. The majority of the swelling will gradually dissipate over the first 3-6 months. You will start to see the true contour of your new abdomen emerge. The numbness around the incision will slowly return, though some altered sensation may be permanent. Your scars will be red, raised, and firm—this is normal. You will begin using scar care treatments (silicone sheets or gel) as directed by your surgeon, usually after the incision is fully healed (around 4-6 weeks). Sun protection (SPF 30+) on the scar is absolutely critical to prevent hyperpigmentation.
Month 6 and Beyond: The Final Reveal
By the 6-month mark, most swelling is resolved, and you can see your panniculectomy final results. The scars will begin to fade, becoming flatter, paler, and softer over the next 12-18 months. At this stage, you can typically resume all normal activities, including vigorous exercise and sports. The functional benefits—freedom from rashes, ease of movement, improved hygiene—are now fully realized. Maintaining a stable weight is paramount to preserve your results.
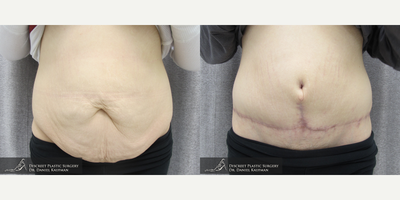
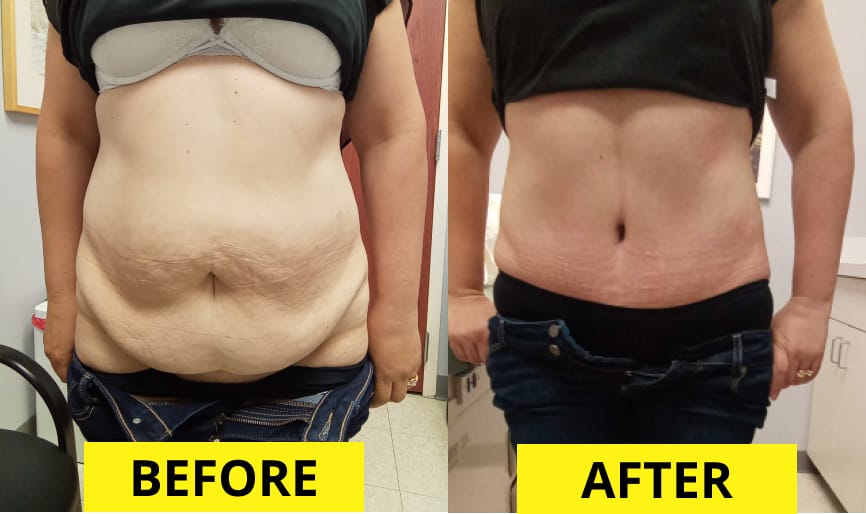
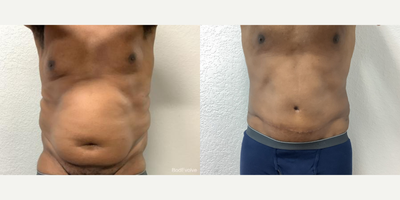
Before and After: The Transformative Evidence
The most powerful testament to this procedure is in the visual and experiential comparison. A panniculectomy before and after gallery shows more than just a flatter belly; it reveals a restored quality of life.
In the "before" photos, you often see:
- A prominent, heavy overhang of skin and fat, sometimes extending to the knees.
- Skin discoloration, darkening (acanthosis nigricans), or chronic irritation and redness in the folds.
- Difficulty standing fully upright, with a constant forward lean to accommodate the weight.
- Clothing that fits poorly, with waistbands digging in or needing to be worn below the pannus.
- A visible sense of discomfort and limitation in the patient’s posture and expression.
In the "after" photos, the transformation is clear:
- A smooth, flat, or gently contoured abdominal profile with a low, discreet scar.
- Elimination of the skin fold and all associated hygiene problems.
- The ability to stand tall and straight with a natural posture.
- Clothing fits the body correctly; patients can wear regular pants and swimwear.
- A visible boost in confidence, often reflected in the patient’s smile and relaxed posture in the photos.
The functional improvement is equally dramatic. Patients report being able to tie their shoes, bend over to garden, exercise without chafing, and experience a level of personal hygiene they hadn’t known in years. The psychological impact of no longer feeling burdened and self-conscious is immense and is a core part of the panniculectomy after results.
Potential Risks and Complications
Like all major surgery, a panniculectomy carries risks. A reputable surgeon will discuss these openly. They include:
- Seroma or Hematoma: Fluid or blood collecting under the skin, the most common complication. Drains help prevent this.
- Infection: Requires antibiotics and possibly drainage.
- Poor Wound Healing: Especially at the ends of the incision (the "dog ears"), which may require minor revision.
- Numbness or Altered Sensation: Usually temporary, but can be permanent around the scar.
- Scarring: All patients will have a permanent scar. Its appearance depends on genetics, wound care, and surgical technique.
- Deep Vein Thrombosis (DVT) and Pulmonary Embolism (PE): Blood clots are a serious risk with any surgery. Early ambulation and sometimes medication are used for prevention.
- Asymmetry: Minor asymmetry can occur, though the goal is a balanced result.
Choosing a board-certified plastic surgeon with extensive experience in body contouring after massive weight loss is the single most important factor in minimizing these risks.
The Cost of a Panniculectomy
The panniculectomy cost varies widely based on geography, surgeon expertise, facility fees, anesthesia, and the extent of the procedure. According to the American Society of Plastic Surgeons, the average surgeon’s fee for a panniculectomy in the United States is approximately $7,000-$9,000. However, this is just the surgeon’s fee. When you add facility costs, anesthesia, and post-operative care, the total package often ranges from $10,000 to $15,000 or more.
Crucially, if the panniculectomy is deemed medically necessary—meaning you have documented recurrent infections, rashes, or mobility issues that have not responded to conservative treatment—insurance may cover a portion or all of the cost. This requires extensive pre-authorization, including letters from your doctor, dermatologist, or primary care physician detailing the medical necessity. A purely cosmetic panniculectomy (performed only for aesthetic reasons with no functional symptoms) is almost always an out-of-pocket expense. Your surgeon’s office can help guide you through the insurance process if applicable.
Real Patient Experiences and Long-Term Satisfaction
Studies and patient surveys consistently show high satisfaction rates for panniculectomy, particularly when performed for functional reasons. A 2020 study in the Aesthetic Surgery Journal reported that over 90% of patients who underwent panniculectomy after massive weight loss were satisfied or very satisfied with their results, citing improvements in hygiene, clothing fit, and physical activity.
Real patient stories highlight the life-changing nature. One patient described being able to walk without waddling for the first time in a decade. Another spoke of the joy of finally being able to shop for clothes in regular stores instead of only in plus-size sections with limited styles. The relief from constant skin infections and the ability to maintain proper hygiene are repeatedly mentioned as life-altering benefits that go far beyond the cosmetic improvement.
Making Your Decision: Is a Panniculectomy Right for You?
Ultimately, the decision to undergo a panniculectomy is deeply personal. Ask yourself:
- Is my pannus causing me physical pain, discomfort, or recurrent medical issues?
- Have I maintained a stable weight for at least a year?
- Am I in good overall health to tolerate anesthesia and surgery?
- Do I understand the scarring and the lengthy recovery process?
- Am I having this surgery for myself, not to please someone else?
If your answers are yes, and the burden of the pannus is diminishing your quality of life, then a panniculectomy could be a profoundly positive step. Schedule consultations with 2-3 board-certified plastic surgeons. Ask to see their panniculectomy before and after photos of patients with a similar body type to yours. Discuss your goals, their recommendations, and the total cost. A good surgeon will make you feel informed, comfortable, and confident in your decision.
Conclusion: Embracing a Lighter, Brighter Future
The journey of a panniculectomy before and after is a testament to the power of modern medicine to restore function and confidence. It is a procedure born from necessity, offering a solution to the very real physical and emotional challenges of living with a large abdominal pannus. The "before" represents a state of burden, limitation, and often discomfort. The "after" represents freedom—freedom of movement, freedom from chronic skin issues, and the freedom to feel comfortable and confident in your own skin.
The road requires patience, with a recovery that unfolds over many months. The result is a permanent, life-changing transformation. If you’ve done the hard work of losing significant weight and are now grappling with the leftover skin, you deserve to reap the full rewards of your achievement. A panniculectomy is not about chasing an unrealistic ideal; it’s about completing your journey to health and reclaiming your body’s functionality and your personal well-being. It’s about finally seeing, in the mirror, the person you’ve worked so hard to become.