Pictures Of Granulation Tissue After Tooth Extraction: A Visual Guide To Normal Healing
Have you ever found yourself squinting at a flashlight, trying to decipher the mysterious landscape inside your mouth a week after a tooth extraction? You’re not alone. Millions of people search for pictures of granulation tissue after tooth extraction every year, driven by a mix of curiosity and concern. Is that red, bumpy tissue normal? Or is it a sign of something worse, like a dry socket? This visual guide will walk you through exactly what you’re looking at, why it’s there, and how to tell the difference between healthy healing and a potential problem. By the end, you’ll be equipped with the knowledge to monitor your own recovery with confidence.
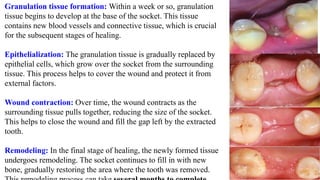
Understanding what happens after a tooth is removed is key to a smooth recovery. The empty socket left behind isn’t just a hole; it’s the starting point for a complex, beautifully orchestrated healing process. One of the most visible—and often misunderstood—stages is the formation of granulation tissue. This article will serve as your comprehensive reference, using descriptive language and comparisons to paint a clear picture when actual images aren’t available. We’ll break down the science, show you what to expect, and provide actionable advice for optimal healing.
What Is Granulation Tissue? The Body’s Natural Repair Kit
The Biology of Healing: From Blood Clot to New Tissue
After your dentist or oral surgeon removes a tooth, the first order of business is to stop the bleeding. A blood clot forms in the alveolar socket (the bony hole where the tooth root was). This clot is crucial—it protects the bone and nerves underneath and serves as a scaffold for new tissue. Within the first 24-48 hours, a fascinating transformation begins. Granulation tissue starts to grow into the socket from the surrounding gum and bone. Think of it as your body’s specialized repair crew, made up of new, delicate blood vessels (angiogenesis), connective tissue cells called fibroblasts, and a temporary extracellular matrix. Its primary job is to rapidly fill the void, deliver oxygen and nutrients, and lay the groundwork for the stronger, more permanent bone and gum tissue that will eventually form.
This tissue is incredibly vascular, meaning it’s filled with tiny, fragile capillaries. That’s why it has its characteristic appearance. It’s a sign that your body’s inflammatory and proliferative phases of healing are proceeding correctly. Without this vital step, the socket would remain an open wound, vulnerable to infection and delayed recovery.
Why It Looks the Way It Does: Red, Bumpy, and Moist
If you could see granulation tissue up close, you’d describe it as reddish-pink, moist, and having a bumpy, granular, or “cobblestone” texture. The vibrant color comes directly from its rich blood supply—it’s essentially a soft, living sponge of new capillaries. The moisture is maintained by a light serous (watery) exudate, which is a normal part of the inflammatory fluid that keeps the area clean and hydrated. The bumpy texture is due to the protruding ends of those new capillaries and the uneven way the tissue initially fills the irregular contours of the socket.
It’s important to note that this tissue is not the same as the dark, firm blood clot that forms immediately after surgery. That initial clot is more gelatinous and dark red or maroon. As granulation tissue invades over 3-7 days, it gradually replaces and absorbs the clot. By the end of the first week, what you often see peeking into the socket is this new, pinker, more textured tissue. It’s a living, developing structure, not a static scab.
- Leaked Mojave Rattlesnakes Secret Lair Found You Wont Believe Whats Inside
- Starzs Ghislaine Maxwell Episodes Leaked Shocking Nude Photos Sex Tapes Exposed
- Skin Club Promo Code
The Role of Pictures in Post-Extraction Care: Why You’re Searching
What Normal Granulation Tissue Looks Like (A Descriptive Guide)
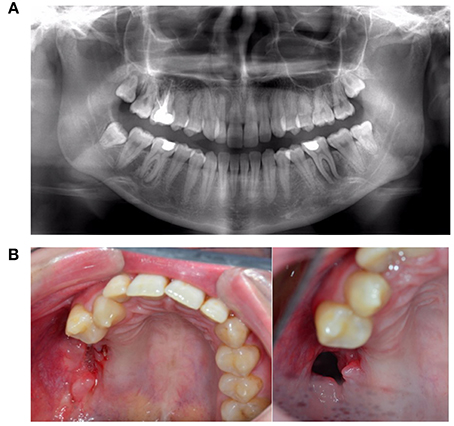
Since you’re reading about pictures of granulation tissue after tooth extraction, let’s create a mental image. Imagine looking into a socket with a good light. A healthy granulation tissue presentation typically includes:
- Color: Bright to medium coral pink, similar to the inside of your lower lip or gums. It should not be bright cherry red (which can indicate inflammation) or dusky purple/gray (a sign of poor blood flow).
- Texture: A shaggy, irregular, pebbled surface. It doesn’t look like smooth skin. It fills the socket unevenly at first.
- Moisture: It has a glossy, wet appearance. Dry, leathery, or chalky tissue is a warning sign.
- Location: It fills the socket from the bottom and sides upward. It should be firmly attached to the surrounding gum tissue. You should not see loose tissue flaps.
- Odor: There should be no foul odor. A mild, metallic smell from blood is normal initially, but it should dissipate.
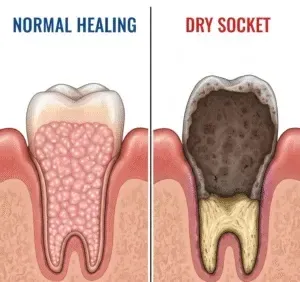
In contrast, an infected socket or dry socket (alveolar osteitis) looks starkly different. Dry socket presents with a dark, empty-looking socket where the clot is missing, exposing bare, grayish bone. The tissue around the edges may be inflamed, but the socket floor is often visible and painful. Infection might show yellow or green pus, significant swelling, and intense, throbbing pain that radiates.
How to Take Your Own Pictures (Safely and Effectively)
If you want to monitor your healing, taking clear pictures can be incredibly useful for your own records and for showing your dentist if concerns arise. Here’s how to do it safely:
- Wash your hands thoroughly with soap and water before and after.
- Use a clean, dry cotton swab or your tongue to gently pull your cheek away from the extraction site. Do not poke or probe the socket itself.
- Use your smartphone’s camera with the flashlight/torch on. The rear camera usually has better quality than the front-facing one.
- Get as close as you can without losing focus. Use the macro or close-up mode if available.
- Take multiple shots from slightly different angles to get the best view of the socket’s depth and sides.
- Do not use Q-tips or fingers to move tissue inside the socket. You risk dislodging the forming clot or introducing bacteria.
- Store the pictures with the date. If you need to consult your dentist, you now have a visual timeline.
Granulation Tissue vs. Signs of Infection: A Critical Comparison
Key Visual Differences: A Side-by-Side Analysis
This is the most common reason for the search. Knowing the difference can prevent unnecessary panic or, conversely, prompt timely care. Let’s compare:
| Feature | Healthy Granulation Tissue | Potential Infection / Dry Socket |
|---|---|---|
| Color | Coral pink, uniform | Dark red/purple, yellow/green (pus), gray (exposed bone) |
| Texture | Moist, bumpy, granular | Dry, leathery, smooth (bone), or mushy with pus |
| Socket Fill | Filling in from bottom/sides | Empty (dry socket) or filled with debris/pus |
| Tissue Edges | Attached, blending with gum | Inflamed, rolled, or separated from socket |
| Odor | None or faint metallic | Foul, rotten, or persistently bad smell |
| Pain Trend | Gradually improving | Worsening after 3-4 days, severe, radiating |
Accompanying Symptoms: What Your Body is Telling You
Visuals are just one part of the diagnostic puzzle. Pay equal attention to how you feel:
- Normal Healing: Discomfort and swelling should peak around day 2-3 and then steadily decrease. Pain is manageable with over-the-counter meds and is localized to the socket.
- Warning Signs (See a dentist immediately):
- Severe, unrelenting pain that starts 3-5 days post-extraction and is not relieved by medication (classic dry socket sign).
- Fever (over 100.4°F or 38°C).
- Swelling that increases after the third day or spreads to the eye or neck.
- Pus or persistent foul taste/odor that doesn’t improve with gentle rinsing.
- Numbness that doesn’t wear off as expected (could indicate nerve involvement).
- Bleeding that restarts heavily after the first 24 hours.
The Healing Timeline: What to Expect Week by Week
Healing is a marathon, not a sprint. Granulation tissue is the star of the first act. Here’s a typical timeline for an uncomplicated extraction:
| Time After Extraction | Primary Healing Activity | What You Might See/Feel |
|---|---|---|
| Day 1-3 | Blood clot formation & initial inflammation. | Dark clot fills socket. Swelling & discomfort peak. |
| Day 4-7 | Granulation tissue proliferation. | Red/pink, bumpy tissue visibly filling socket. Pain/swelling decrease. |
| Week 2-3 | Granulation tissue matures; early bone formation begins. | Socket appears much smaller. Tissue becomes less red, more pink. |
| Week 4-6 | Bone mineralization and gum tissue closure. | Socket is 60-80% filled with new bone. Gum tissue grows over the top. |
| Month 2-6 | Bone remodeling and maturation. | Socket fills completely with dense bone. Gum line returns to near-normal. |
Important Note: This timeline varies based on extraction complexity (simple vs. surgical), your age, overall health, and adherence to aftercare instructions. A surgical extraction (with bone removal or stitches) will have a longer, more involved healing process with more pronounced granulation tissue initially.
Factors That Influence Granulation Tissue Formation and Healing
Your body’s ability to produce healthy granulation tissue isn’t uniform. Several factors play a decisive role:
- Systemic Health: Conditions like uncontrolled diabetes, immunocompromising disorders (e.g., HIV, chemotherapy), and vascular disease impair blood flow and cell regeneration, slowing granulation.
- Lifestyle Factors:Smoking and tobacco use is the single biggest modifiable risk factor. Nicotine causes vasoconstriction (narrows blood vessels), drastically reducing blood flow to the socket and leading to delayed granulation, increased infection risk, and higher dry socket rates (up to 30% in smokers vs. 2-5% in non-smokers).
- Oral Hygiene: Gentle rinsing with salt water or prescribed mouthwash after the first 24 hours keeps the area clean without disrupting the clot. Poor hygiene invites bacteria that can overwhelm the healing tissue.
- Nutrition: Your body needs protein, Vitamin C, zinc, and calcium to build new tissue. A poor diet starves the healing process.
- Trauma to the Site: Aggressive rinsing, spitting, sucking through straws, or poking the socket with your tongue or finger can dislodge the fragile clot and nascent granulation tissue, setting healing back to square one.
- Medications:Bisphosphonates (for osteoporosis) or anti-angiogenic drugs (some cancer treatments) can impair bone healing and granulation tissue formation. Always disclose your full medical history.
Essential Aftercare Tips to Promote Healthy Granulation Tissue
Your actions in the first 72 hours are critical. Follow these evidence-based tips to foster the perfect environment for granulation tissue to thrive:
- Protect the Clot (First 24 Hours): Bite firmly on the gauze pad provided. Avoid rinsing, spitting, or drinking through a straw. This allows the initial clot to stabilize.
- Gentle Rinsing (After 24 Hours): Use a saltwater rinse (1/2 teaspoon salt in 8oz warm water) 3-4 times a day, especially after meals. Swish gently and let it fall out—do not vigorously gargle. This cleanses without disrupting tissue.
- Diet: Stick to soft, cool foods for the first few days (yogurt, applesauce, mashed potatoes, smoothies). Avoid hot, spicy, crunchy, or chewy foods that can irritate the socket or get trapped.
- Hydration: Drink plenty of water, but avoid carbonated beverages and alcohol for at least a week.
- Oral Hygiene:Brush your teeth normally, but avoid the immediate extraction site for the first 24 hours. After that, brush gently, avoiding direct scrubbing on the socket. You can use a soft-bristled child’s toothbrush for better control.
- No Smoking:Do not smoke for at least 72 hours, but ideally a full week. The negative impact on blood flow is immediate and severe.
- Rest and Elevation: Avoid strenuous exercise for 2-3 days. Keep your head elevated with pillows while resting to reduce swelling and bleeding.
- Pain Management: Take prescribed or recommended pain medication as directed. Controlling pain helps you avoid disruptive habits like poking the area.
When to Contact Your Dentist: Recognizing the Red Flags
While granulation tissue is a welcome sight, certain developments require professional intervention. Do not wait. Call your dentist or oral surgeon immediately if you experience:
- Uncontrolled bleeding that persists after 1-2 hours of firm pressure with gauze.
- Severe pain that worsens after the third day and is not relieved by your prescribed pain medication (classic symptom of dry socket).
- Swelling that increases after the third day, especially if it involves your eye, cheek, or the floor of your mouth.
- Difficulty breathing or swallowing (a medical emergency—go to ER).
- Pus or a persistent foul taste/odor that doesn’t improve with rinsing.
- Fever of 100.4°F (38°C) or higher.
- Numbness in the lip, chin, or tongue that doesn’t gradually return (could indicate nerve irritation).
- Any feeling that “something isn’t right.” Trust your instincts. It’s always better to have a professional reassure you or treat a complication early.
Conclusion: Your Healing Journey, Demystified
Searching for pictures of granulation tissue after tooth extraction is a smart, proactive step in taking control of your oral health recovery. That red, bumpy, moist tissue filling your socket is not a cause for alarm—it’s a visual testament to your body’s remarkable healing capacity. It’s the vibrant, vascular scaffold upon which strong bone and gum will be built. By understanding its appearance, its role in the healing timeline, and the critical difference between this healthy tissue and signs of infection, you transform anxiety into informed observation.
Remember, healing is not linear. Some days the socket might look different, and that’s normal as tissue matures and contracts. Your primary guides are trend and accompanying symptoms: is pain decreasing? Is swelling going down? Is there no fever or foul odor? If the answer is yes, that granulation tissue is doing its job perfectly. Arm yourself with the aftercare strategies outlined, avoid the major disruptors like smoking and probing, and you create the optimal conditions for seamless repair. And when in doubt, that’s what your dental team is for—a quick phone call or photo review can provide peace of mind and ensure any true complication is addressed swiftly. Your journey from extraction to full recovery is now a little less mysterious.